What is Multiple Sclerosis?
Multiple Sclerosis is an autoimmune disorder that affects the central nervous system (CNS). When a person has an autoimmune disease, the immune system attacks healthy tissue, just as it might attack a virus or bacteria. In the case of MS, the immune system attacks the myelin sheath that surrounds and protects the nerve fibers, causing inflammation. Myelin allows the nerves to conduct electrical signals quickly and efficiently.
Multiple sclerosis means “scar tissue in multiple areas.”
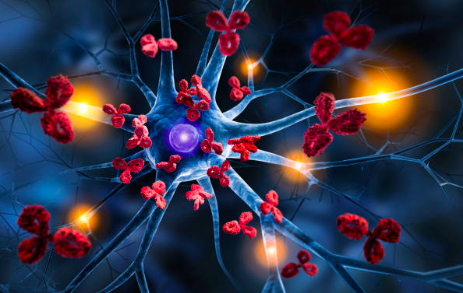
This mainly affects:
- the brain stem
- the cerebellum, which coordinates movement and controls balance
- the spinal cord
- the optic nerves
- white matter in some regions of the brain
As more lesions develop, nerve fibers can break or become damaged. As a result, the electrical impulses from the brain do not flow smoothly to the target nerve. This means that the body cannot carry out certain functions.
4 types of Multiple Sclerosis:
- Clinically isolated syndrome (CIS):
This is a single, first episode, with symptoms lasting at least 24 hours. If another episode occurs at a later date, a doctor might diagnose relapse-remitting MS.
- Relapse-remitting MS (RRMS):
This is the most common form. Around 85% of people with MS are initially diagnosed with RRMS. RRMS involves episodes of new or increasing symptoms, followed by periods of remission, during which symptoms go away partially or totally.
- Primary progressive MS (PPMS):
Symptoms worsen progressively, without early relapses or remissions. Some people may experience times of stability and periods when symptoms worsen and then get better. Around 15% of people with MS have PPMS.
- Secondary progressive MS (SPMS):
At first, people will experience episodes of relapse and remission, but then the disease will start to progress steadily.
Symptoms:
- Muscle weakness: People may develop weak muscles due to lack of use or stimulation due to nerve damage.
- Numbness and tingling: A pins and needles-type sensation is one of the earliest symptoms of MS and can affect the face, body, arms, and legs.
- Lhermitte’s sign: A person may experience a sensation like an electric shock when they move their neck, known as Lhermitte’s sign.
- Bladder problems: A person may have difficulty emptying their bladder or need to urinate frequently or suddenly, known as urge incontinence. Loss of bladder control is an early sign of MS.
- Bowel problems: Constipation can cause fecal impaction, which can lead to bowel incontinence.
- Fatigue: This can undermine a person’s ability to function at work or at home, and is one of the most common symptoms of MS.
- Dizziness and vertigo: These are common problems, along with balance and coordination issues.
- Sexual dysfunction: Both males and females may lose interest in sex.
- Spasticity and muscle spasms: This is an early sign of MS. Damage to nerve fibers in the spinal cord and brain can cause painful muscle spasms, including in the legs.
It also includes:
- Tremor: Some people with MS may experience involuntary quivering movements.
- Vision problems: Some people may experience double or blurred vision or a partial or total loss of vision. This usually affects one eye at a time. Inflammation of the optic nerve can result in pain when the eye moves. Vision problems are an early sign of MS.
- Gait and mobility changes: MS can change the way people walk due to muscle weakness and problems with balance, dizziness, and fatigue.
- Emotional changes and depression: Demyelination and nerve fiber damage in the brain can trigger emotional changes.
- Learning and memory problems: These can make it difficult to concentrate, plan, learn, prioritize, and multitask.
- Pain: Pain is a common symptom in MS. Neuropathic pain is directly due to MS, while muscle spasticity or stiffness may cause localized pain.

Treatment:
There is currently no cure for MS:
Treatment focuses on managing symptoms, reducing relapses (periods when symptoms worsen) and slowing the disease’s progression. Your comprehensive treatment plan may include:
- Disease-modifying therapies (DMTs): Several medications have FDA approval for long-term MS treatment. These drugs help reduce relapses (also called flare-ups or attacks). They slow down the disease’s progression. And they can prevent new lesions from forming on the brain and spinal cord.
- Relapse management medications:
If you have a severe attack, your neurologist may recommend a high dose of corticosteroids. The medication can quickly reduce inflammation. They slow damage to the myelin sheath surrounding your nerve cells.
- Physical rehabilitation:
Multiple sclerosis can affect your physical function. Staying physically fit and strong will help you maintain your mobility.
- Mental health counseling:
Coping with a chronic condition can be emotionally challenging. And MS can sometimes affect your mood and memory. Working with a neuropsychologist or getting other emotional support is an essential part of managing the disease.





Great post. I am facing a couple of these problems.
I can be your obedient free online live adult webcams or, if you need a powerful mistress
I am open, humorous and outgoing. Dominant by nature. I am looking for free live sex cams to entertain me, I enjoy watching you give me a horny show with your fetish.