Glenn Procedure: How It Works, Benefits & Risks
The Glenn procedure, named after its pioneering creator, Dr. William Glenn, is a surgical intervention used to treat complex congenital heart defects. This intricate procedure plays a vital role in providing improved blood flow to the lungs. It ensures better oxygenation of the blood, and ultimately enhancing the overall quality of life. This is mostly for individuals born with specific heart conditions. In this comprehensive exploration, we delve into the intricacies of the Glenn procedure. We will understand its medical applications and the impact it has. Especially, on the lives of those affected by congenital heart defects.
Medical Applications of the Glenn Procedure
The Glenn procedure primarily occurs or takes place in the management of congenital heart defects. These ones affect the circulation of blood between the heart and the lungs. Specifically, it’s utilisation is for cases where a single ventricle or other complex heart anomalies make it impossible for the heart to pump blood. The heart is unable to pump effectively to both the body and the lungs. The procedure redirects some of the blood that would normally flow to the lungs directly into the pulmonary artery. Thus it improves oxygenation.
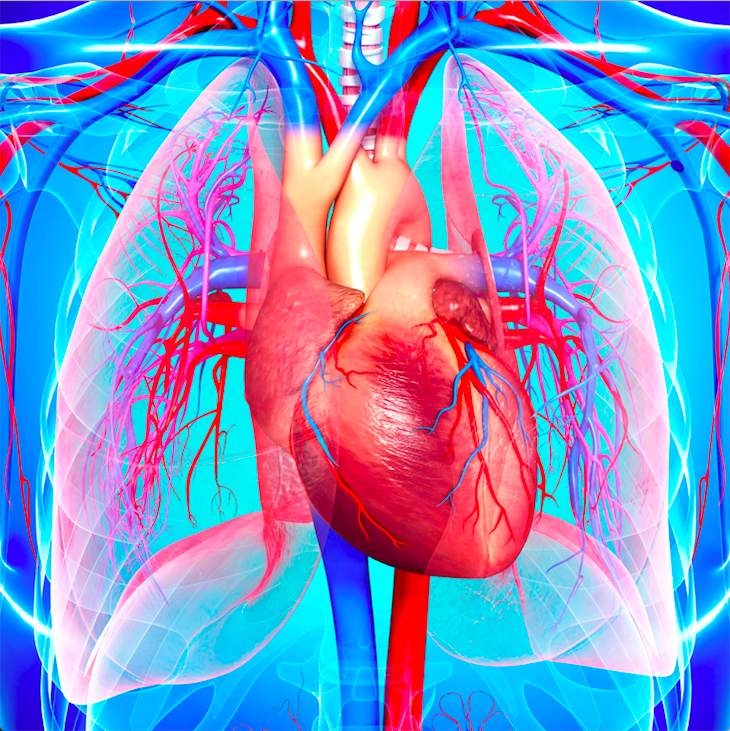
Here’s a simplified overview of how the Glenn procedure works:
- Patient Preparation: The patient, often an infant or young child, is prepared for surgery. General anesthesia is administered, and the surgical team monitors vital signs throughout the procedure.
- Accessing the Heart: A small incision in the chest takes place, and the surgeon gains access to the heart and its major blood vessels. The patient may have a connection line to a heart-lung machine to ensure that blood continues to circulate while the procedure is underway.
- Creating the Connection: Using intricate surgical techniques, the surgeon creates a direct connection between the superior vena cava (the major vein carrying deoxygenated blood from the upper body) and the pulmonary artery (the blood vessel that carries oxygen-poor blood to the lungs).
- Redirecting Blood Flow: With this connection in place, a portion of the deoxygenated blood from the upper body undergoes diversion to the pulmonary artery. This “bypass” reduces the workload on the heart and ensures better oxygenation of the blood.
- Closure and Recovery: Once the connection is secure, the surgical team carefully closes the incision. The patient laters weans off the heart-lung machine and monitored during the initial stages of recovery.
Benefits and Considerations
The Glenn procedure offers several significant benefits for patients with the aforementioned congenital heart defects:
- Improved Oxygenation: By redirecting blood flow directly to the pulmonary artery, the procedure enhances the oxygenation of blood without increasing the workload on the heart.
- Enhanced Quality of Life: Many children who undergo the Glenn procedure experience improved energy levels, reduced symptoms of heart failure, and an overall better quality of life.
- Staging for Complex Repairs: In some cases, the Glenn procedure is the first step in a staged approach to address complex heart defects. It allows the patient to grow and gain strength before undergoing further surgical interventions.
- Reduced Cyanosis: Cyanosis, a bluish discoloration of the skin and mucous membranes due to insufficient oxygen in the blood, is often alleviated following the Glenn procedure.
However, it’s essential to understand that the Glenn procedure is not a complete cure for congenital heart defects. It is a palliative measure that helps manage the condition and improve the patient’s overall health, but additional surgeries or interventions may be necessary as the child grows.
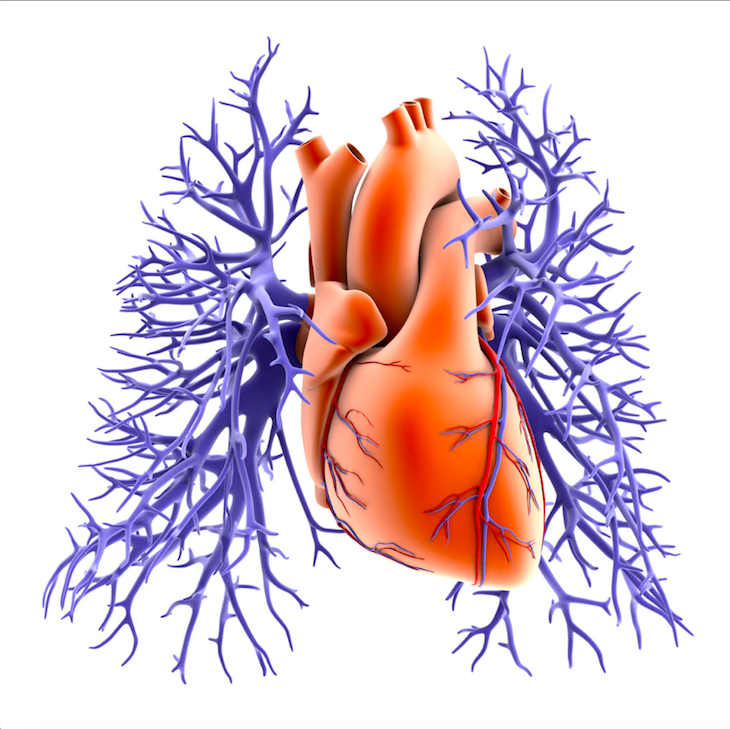
Challenges and Risks
Like any surgical procedure, the Glenn procedure carries inherent risks, and the decision to proceed with it is a careful decision, weighing the potential benefits against these risks. Some of the challenges and risks associated with the Glenn procedure include:
- Bleeding: There is a risk of bleeding, which closely undergoes monitioring during and after the procedure.
- Infection: Surgical site infections can occur, although strict sterile techniques are available to minimize this risk.
- Blood Clots: The manipulation of blood vessels can increase the risk of blood clots. This can potentially lead to serious complications.
- Arrhythmias: Irregular heart rhythms may develop, requiring further treatment or intervention.
- Fluid Accumulation: Accumulation of fluid around the heart (pericardial effusion) or in the lungs (pleural effusion) is possible.
- Residual or Recurrent Defects: In some cases, residual or recurrent heart defects may necessitate additional surgeries.
- Long-Term Follow-Up: Patients who undergo the Glenn procedure require long-term monitoring by a pediatric cardiologist. The cardiologist to assesses their heart function and overall health.
Despite these potential challenges, the Glenn procedure has transformed the prognosis for children born with specific congenital heart defects. This offers them a chance at a healthier and more fulfilling life.





Que Contiene El Cialis
I am very grateful to you for the information.
Cialis 5 mg prezzo prezzo cialis 5 mg originale in farmacia tadalafil 5 mg prezzo
OpenAI,ChatGPT: A Year of Unprecedented Evolution in AI Conversational Technology
renowned for its significant contributions in the realm of AI research and development, took an astronomical leap into the limelight with the monumental launch of ChatGPT in November 2022. What followed in the ensuing twelve months has been nothing short of a fascinating odyssey, transforming the landscape of human-AI interactions.
кэт казино
7sps.ru
It’s amazing to visit this web site and reading the views of all friends regarding this paragraph, while I am also keen of getting knowledge.
My page site#:
http://molbiol.ru/forums/index.php?showtopic=1085471
http://zorkiy.bestbb.ru/viewtopic.php?id=157#p164
http://realniemoney.0pk.me/viewtopic.php?id=3824#p9144
https://woke.party/blogs/104729/Путь-к-успеху-или-выражение-личной-инициативы-Покупка-диплома-рассматривается
https://lolka.bestbb.ru/viewtopic.php?id=533#p3890
vegas grand официальный сайт казино
вегас гранд казино регистрация с выводом
Aviator Spribe регистрация казино
I think, that you are not right. I am assured. Let’s discuss. Write to me in PM, we will communicate.
Добро пожаловать в захватывающий мир авиаторов! Aviator – это увлекательная игра, которая позволит вам окунуться в атмосферу боевых действий на небе. Необычные графика и захватывающий сюжет сделают ваше путешествие по воздуху неповторимым.
Играйте в автомат Aviator Spribe казино играть с друзьями и ощутите волнение азарта!
Aviator игра позволит вам почувствовать себя настоящим пилотом. Вам предстоит совершить невероятные маневры, выполнять сложные задания и сражаться с противниками. Улучшайте свой самолет, чтобы быть готовым к любым ситуациям и становиться настоящим мастером.
Основные особенности Aviator краш игры:
1. Реалистичная графика и физика – благодаря передовой графике и реалистичной физике вы почувствуете себя настоящим пилотом.
2. Разнообразные режимы игры и миссии – в Aviator краш игре вы сможете выбрать различные режимы игры, такие как гонки, симулятор полетов и захватывающие воздушные бои. Кроме того, каждая миссия будет предлагать свои собственные вызовы и задачи.
3. Улучшение и модернизация самолетов – в игре доступны различные модели самолетов, которые можно покупать и улучшать. Вы сможете устанавливать новое оборудование, улучшать двигательность и мощность своего самолета, а также выбирать различные варианты окраски и декорации.
Aviator краш игра – это возможность испытать себя в роли авиатора и преодолеть все сложности и опасности воздушного пространства. Почувствуйте настоящую свободу и адреналин в Aviator краш игре онлайн!
Играйте в «Авиатор» в онлайн-казино Pin-Up
Aviator краш игра онлайн предлагает увлекательную и захватывающую игровую атмосферу, где вы становитесь настоящим авиатором и сражаетесь с самыми опасными искусственными интеллектами.
В этой игре вы должны показать свое мастерство и смекалку, чтобы преодолеть сложности многочисленных локаций и уровней. Вам предстоит собирать бонусы, уклоняться от препятствий и сражаться с врагами, используя свои навыки пилотирования и стрельбы.
Каждый уровень игры Aviator краш имеет свою уникальную атмосферу и задачи. Будьте готовы к неожиданностям, так как вас ждут захватывающие повороты сюжета и сложные испытания. Найдите все пути к победе и станьте настоящим героем авиатором!
Авиатор игра является прекрасным способом провести время и испытать настоящий адреналиновый разряд. Готовы ли вы стать лучшим авиатором? Не упустите свой шанс и начните играть в Aviator краш прямо сейчас!
Aviator – играй, сражайся, побеждай!
Aviator Pin Up (Авиатор Пин Ап ) – игра на деньги онлайн Казахстан
Aviator игра предлагает увлекательное и захватывающее разнообразие врагов и уровней, которые не оставят равнодушными даже самых требовательных геймеров.
Враги в Aviator краш игре онлайн представлены в самых разных формах и размерах. Здесь вы встретите группы из маленьких и быстрых врагов, а также огромных боссов с мощным вооружением. Разнообразие врагов позволяет игрокам использовать разные тактики и стратегии для победы.
Кроме того, Aviator игра предлагает разнообразие уровней сложности. Выберите легкий уровень, чтобы насладиться игровым процессом, или вызовите себе настоящий вызов, выбрав экспертный уровень. Независимо от выбранного уровня сложности, вы получите максимум удовольствия от игры и окунетесь в захватывающий мир авиаторов.
Играйте в Aviator и наслаждайтесь разнообразием врагов и уровней, которые позволят вам почувствовать себя настоящим авиатором.
Hi there colleagues, how is all, and what you would like to say about this article, in my view its genuinely amazing for me.
http://www.google.com.mx/url?q=https://hottelecom.biz/id/
#Best #site #awords:
koop een virtueel telefoonnummer
аренда виртуального номера
Наша компания предлагает полный спектр услуг по ремонту и отделке Квартир, коттеджей и домов под ключ в Алматы. Мы берем на себя все этапы работы, начиная с разработки дизайн-проекта и заканчивая финальной отделкой и установкой мебели. В нашем пакете услуг входит: Отделка и Ремонт Загородного Дома под ключ в Алматы
Авиатор Спрайб играть на рубли
Добро пожаловать в захватывающий мир авиаторов! Aviator – это увлекательная игра, которая позволит вам окунуться в атмосферу боевых действий на небе. Необычные графика и захватывающий сюжет сделают ваше путешествие по воздуху неповторимым.
Aviator Spribe казино играть на евро
Howdy I am so glad I found your weblog, I really found you by mistake, while I was browsing on Google for something else, Nonetheless I am here now and would just like to say many thanks for a remarkable post and a all round enjoyable blog (I also love the theme/design), I don’t have time to read through it all at the moment but I have saved it and also added your RSS feeds, so when I have time I will be back to read a great deal more, Please do keep up the superb work.
RybelsusRybelsusRybelsusRybelsusRybelsus
What’s up everyone, it’s my first visit at this web site, and post is really fruitful designed for me, keep up posting these posts.
Rybelsus
Keep this going please, great job!
writing service
Завод из России продает разборные гантели https://gantel-razbornaya.ru/ – у нас найдете обширный каталог предложений. Комфортные снаряды дают продуктивно выполнять силовые занятия в любом месте. Спортивные снаряды отличаются удобством, универсальностью в эксплуатации. Компания из России продуктивно изучает и внедряет свежие идеи, чтобы осуществить спортивные цели постоянных покупателей. В выпуске долговечных отягощений всегда применяются лучшие марки чугуна. Широкий набор моделей позволяет приобрести удобные утяжелители для эффективной программы занятий. Для домашних тренировок – это комфортный инвентарь с компактными габаритами и значительной фунциональности.
Производимые отечественной компанией тренажеры для кинезитерапии https://trenazhery-dlya-kineziterapii.ru и специально разработаны для восстановления после травм. Устройства имеют лучшее предложение цены и качества.
Продаем очень недорого Кроссовер с перекрестной тягой с облегченной конструкцией. В каталоге интернет-магазина для кинезитерапии всегда в реализации варианты блочного и нагружаемого типа.
Изготавливаемые тренажеры для реабилитации обеспечивают мягкую и безопасную тренировку, что особенно важно для тренирующихся пациентов в процессе восстановления.
Конструкции обладают изменяемым сопротивлением и уровнями нагрузки, что дает возможность индивидуализировать тренировки в соответствии с задачами любого пациента.
Все устройства подходят для кинезитерапии по руководству профессора Сергея Бубновского. Оборудованы поручнями для удобного осуществления тяг в наклоне или лежа.
Wow that was strange. I just wrote an incredibly long comment but after I clicked submit my comment didn’t show up. Grrrr… well I’m not writing all that over again. Anyway, just wanted to say excellent blog!
http://cad1.co.kr/bbs/board.php?bo_table=free&wr_id=374906
Its like you read my mind! You seem to know a lot about this, like you wrote the book in it or something. I think that you could do with a few pics to drive the message home a bit, but instead of that, this is fantastic blog. An excellent read. I’ll definitely be back.
Официальный сайт Гама казино
Gama casino
What’s up, after reading this amazing post i am also delighted to share my know-how here with colleagues.
Gama casino
Здравствуйте!
Вы когда-нибудь сталкивались с необходимостью написания дипломной работы в сжатые сроки? Это действительно очень ответственное и трудоемкое занятие, но важно не опускать руки и продолжать двигаться вперед, активно занимаясь учебным процессом, как и я.
Для тех, кто умеет находить и анализировать информацию в сети, это действительно помогает в процессе согласования и написания дипломной работы. Больше не нужно тратить время на посещение библиотек или организацию встреч с научным руководителем. Именно здесь, на этом ресурсе, можно найти надежные данные для заказа и написания дипломных и курсовых работ с гарантией качества и доставкой по всей России. Можете ознакомиться с предложениями на [url=https://rudik-diploms365.com/]купить диплом колледжа[/url], это проверенный источник!
https://gruppa365-diploms-srednee.com/
купить диплом магистра
купить диплом бакалавра
купить диплом специалиста
купить диплом нового образца
купить диплом
Желаю любому прекрасных отметок!
Приветики!
Вы когда-нибудь сталкивались с необходимостью написания дипломной работы в сжатые сроки? Это действительно очень ответственное и трудоемкое занятие, но важно не опускать руки и продолжать двигаться вперед, активно занимаясь учебным процессом, как и я.
Для тех, кто умеет находить и анализировать информацию в сети, это действительно помогает в процессе согласования и написания дипломной работы. Больше не нужно тратить время на посещение библиотек или организацию встреч с научным руководителем. Именно здесь, на этом ресурсе, можно найти надежные данные для заказа и написания дипломных и курсовых работ с гарантией качества и доставкой по всей России. Можете ознакомиться с предложениями на [url=https://rudik-diploms365.com/]купить диплом о высшем образовании[/url], это проверенный источник!
https://landik-diploms-srednee24.com/
купить диплом специалиста
купить диплом цена
купить диплом института
где купить диплом
купить аттестат
Желаю каждому положительных отметок!
Earnestcub
Приветики, дорогие мои!!
Продолжаю трудиться над дипломом, несмотря на все трудности, и благодарен сети за предоставленные ресурсы.
Желаете заказать и купить диплом ВУЗа недорого без предоплаты на нашем сайте? Доставим в любую точку России.
Желаю вам всем не двоешных) оценок!
купить свидетельство о рождении ссср
купить диплом в новошахтинске
купить диплом в сызрани
купить диплом в майкопе
купить диплом в арзамасе
купить диплом гознак
купить диплом мастера маникюра и педикюра
купить диплом в комсомольске-на-амуре
купить диплом менеджера
купить диплом в ессентуках
Доброго всем дня!
Закажите диплом Вуза с гарантией качества и доставкой по всей России без предоплаты.
https://image.google.as/url?q=https://russian-diplom.com
https://www.google.me/url?q=http://russdiplomiki.com
https://www.google.ac/url?q=https://russian-diplom.com
https://clients1.google.com.hk/url?sa=t&url=http://free-diplommi.com
https://clients1.google.lv/url?sa=t&url=https://russian-diplom.com
У нас вы можете заказать документы об образовании всех ВУЗов России с доставкой по РФ и оплатой после получения – просто и удобно!
Earnestcub
Добрый день!
Моя борьба с дипломом обернулась настоящим кошмаром, но я не сдаюсь благодаря полезным материалам, обнаруженным в интернете.
Купите диплом у нас легко! Надежно, качественно, без предоплаты, с доставкой в любой город России.
Желаю для каждого прекрасных отметок!
купить диплом в елабуге
купить диплом геодезиста
купить диплом в туймазы
купить диплом в мытищах
купить диплом в салавате
купить диплом в бугульме
купить диплом отзывы
купить диплом в севастополе
купить диплом в томске
купить диплом в копейске
Earnestcub
Привет всем!
Диплом остается в центре моего внимания, но теперь я вооружен необходимыми онлайн-инструментами для его успешного завершения.
У нас вы можете приобрести диплом университета без предоплаты, с доставкой по всей России.
Желаю каждому честных оценок!
купить диплом физика
купить диплом эколога
купить диплом автомеханика
купить диплом охранника
купить свидетельство о рождении ссср
купить диплом в балашихе
купить диплом биолога
купить диплом в грозном
купить диплом в озёрске
где купить диплом образование
Your place is valueble for me. Thanks!…
В нашем обществе, где диплом – это начало отличной карьеры в любом направлении, многие пытаются найти максимально быстрый и простой путь получения качественного образования. Наличие официального документа об образовании переоценить невозможно. Ведь именно диплом открывает дверь перед всеми, кто стремится вступить в профессиональное сообщество или продолжить обучение в высшем учебном заведении.
Наша компания предлагает быстро получить любой необходимый документ. Вы можете приобрести диплом старого или нового образца, и это будет выгодным решением для человека, который не смог закончить обучение или потерял документ. диплом изготавливается с особой аккуратностью, вниманием ко всем деталям, чтобы в результате получился продукт, максимально соответствующий оригиналу.
Превосходство подобного подхода состоит не только в том, что вы быстро получите диплом. Процесс организовывается удобно и легко, с профессиональной поддержкой. От выбора необходимого образца до консультации по заполнению персональной информации и доставки по стране — все находится под абсолютным контролем качественных специалистов.
Таким образом, всем, кто ищет быстрый способ получения необходимого документа, наша компания может предложить выгодное решение. Купить диплом – значит избежать длительного обучения и сразу перейти к достижению собственных целей, будь то поступление в университет или старт карьеры.
https://dlplomanrussian.com
В современном мире, где диплом становится началом отличной карьеры в любом направлении, многие стараются найти максимально быстрый и простой путь получения образования. Факт наличия официального документа об образовании переоценить попросту невозможно. Ведь диплом открывает дверь перед всеми, кто желает начать трудовую деятельность или учиться в высшем учебном заведении.
Наша компания предлагает максимально быстро получить этот важный документ. Вы сможете купить диплом, что становится отличным решением для человека, который не смог закончить обучение или потерял документ. Все дипломы изготавливаются с особой тщательностью, вниманием ко всем нюансам, чтобы на выходе получился полностью оригинальный документ.
Преимущества этого решения состоят не только в том, что можно максимально быстро получить диплом. Весь процесс организован удобно, с нашей поддержкой. Начав от выбора нужного образца документа до консультации по заполнению персональных данных и доставки по России — все находится под абсолютным контролем квалифицированных мастеров.
Всем, кто ищет оперативный способ получить необходимый документ, наша компания предлагает выгодное решение. Купить диплом – это значит избежать долгого обучения и сразу переходить к достижению личных целей, будь то поступление в университет или старт карьеры.
https://dlplomanrussian.com
ShaneAdoks
Всем хорошего дня!
Диплом требует множество усилий, но интернет значительно облегчает этот процесс.
Наша компания поможет вам купить диплом ВУЗа со скидкой и гарантированной доставкой по всей стране.
Желаю для каждого отличных оценок!
купить диплом в камышине
купить диплом в сочи
купить диплом в кузнецке
купить диплом в арзамасе
купить диплом во владимире
купить диплом в заречном
купить диплом в верхней пышме
купить диплом в кургане
купить диплом в новоалтайске
купить диплом в ессентуках
В нашем обществе, где диплом становится началом отличной карьеры в любом направлении, многие пытаются найти максимально быстрый и простой путь получения образования. Факт наличия документа об образовании сложно переоценить. Ведь именно диплом открывает дверь перед всеми, кто желает вступить в профессиональное сообщество или учиться в ВУЗе.
В данном контексте наша компания предлагает очень быстро получить этот важный документ. Вы сможете заказать диплом, что будет удачным решением для всех, кто не смог завершить обучение, утратил документ или хочет исправить свои оценки. дипломы изготавливаются аккуратно, с максимальным вниманием ко всем нюансам. На выходе вы получите документ, полностью соответствующий оригиналу.
Превосходство такого подхода заключается не только в том, что можно максимально быстро получить свой диплом. Весь процесс организован просто и легко, с нашей поддержкой. От выбора нужного образца до консультаций по заполнению личной информации и доставки по стране — все будет находиться под полным контролем наших мастеров.
Всем, кто пытается найти оперативный способ получения требуемого документа, наша компания готова предложить отличное решение. Приобрести диплом – это значит избежать длительного процесса обучения и сразу переходить к достижению личных целей, будь то поступление в университет или старт карьеры.
https://clients1.google.no/url?sa=t&url=https://lands-diploma.com
https://www.google.md/url?sa=t&url=https://lands-diploma.com
https://images.google.com.kh/url?q=https://lands-diploma.com
http://www.google.com.ar/url?q=https://rudiplomista.com
http://www.google.co.ao/url?q=https://lands-diploma.com
В нашем обществе, где диплом является началом удачной карьеры в любом направлении, многие стараются найти максимально быстрый и простой путь получения качественного образования. Факт наличия официального документа трудно переоценить. Ведь именно диплом открывает двери перед всеми, кто хочет начать профессиональную деятельность или учиться в высшем учебном заведении.
В данном контексте наша компания предлагает оперативно получить любой необходимый документ. Вы сможете заказать диплом нового или старого образца, и это является отличным решением для всех, кто не смог завершить образование или утратил документ. Все дипломы выпускаются аккуратно, с максимальным вниманием ко всем элементам. На выходе вы получите полностью оригинальный документ.
Плюсы подобного решения состоят не только в том, что вы быстро получите диплом. Весь процесс организован просто и легко, с нашей поддержкой. От выбора нужного образца до правильного заполнения личных данных и доставки в любое место страны — все будет находиться под полным контролем квалифицированных специалистов.
Всем, кто ищет оперативный способ получить необходимый документ, наша компания предлагает выгодное решение. Заказать диплом – значит избежать долгого процесса обучения и сразу переходить к достижению собственных целей, будь то поступление в университет или начало профессиональной карьеры.
https://diploman-russiyan.com
Сегодня, когда диплом является началом удачной карьеры в любой области, многие ищут максимально быстрый и простой путь получения качественного образования. Наличие официального документа об образовании переоценить просто невозможно. Ведь именно диплом открывает двери перед каждым человеком, желающим вступить в сообщество профессиональных специалистов или продолжить обучение в университете.
Предлагаем оперативно получить этот необходимый документ. Вы можете приобрести диплом нового или старого образца, что будет выгодным решением для человека, который не смог закончить образование, потерял документ или хочет исправить свои оценки. дипломы изготавливаются с особой тщательностью, вниманием ко всем элементам. На выходе вы получите полностью оригинальный документ.
Преимущества такого подхода состоят не только в том, что можно максимально быстро получить диплом. Процесс организовывается комфортно, с профессиональной поддержкой. Начиная от выбора нужного образца документа до точного заполнения личной информации и доставки по стране — все находится под полным контролем квалифицированных специалистов.
Всем, кто пытается найти быстрый и простой способ получения требуемого документа, наша услуга предлагает отличное решение. Заказать диплом – это значит избежать длительного процесса обучения и не теряя времени переходить к своим целям, будь то поступление в ВУЗ или начало профессиональной карьеры.
https://diploman-rossiya.com
В современном мире, где диплом становится началом удачной карьеры в любом направлении, многие пытаются найти максимально простой путь получения образования. Факт наличия официального документа об образовании сложно переоценить. Ведь диплом открывает двери перед всеми, кто собирается вступить в профессиональное сообщество или учиться в ВУЗе.
В данном контексте наша компания предлагает очень быстро получить любой необходимый документ. Вы имеете возможность купить диплом старого или нового образца, и это становится отличным решением для человека, который не смог закончить образование, потерял документ или желает исправить плохие оценки. дипломы изготавливаются аккуратно, с максимальным вниманием ко всем элементам, чтобы в итоге получился продукт, 100% соответствующий оригиналу.
Плюсы данного подхода состоят не только в том, что вы быстро получите свой диплом. Весь процесс организовывается комфортно и легко, с нашей поддержкой. От выбора необходимого образца документа до консультаций по заполнению персональной информации и доставки по России — все находится под абсолютным контролем качественных специалистов.
Для всех, кто хочет найти быстрый и простой способ получить необходимый документ, наша компания предлагает выгодное решение. Купить диплом – значит избежать длительного обучения и не теряя времени перейти к достижению личных целей, будь то поступление в ВУЗ или старт карьеры.
https://diploman-russiyans.com
В современном мире, где диплом – это начало успешной карьеры в любом направлении, многие ищут максимально быстрый и простой путь получения качественного образования. Наличие официального документа переоценить невозможно. Ведь диплом открывает дверь перед людьми, стремящимися вступить в сообщество профессиональных специалистов или учиться в ВУЗе.
Наша компания предлагает оперативно получить этот необходимый документ. Вы имеете возможность купить диплом нового или старого образца, и это является отличным решением для всех, кто не смог завершить образование или потерял документ. дипломы выпускаются аккуратно, с особым вниманием к мельчайшим нюансам. В итоге вы сможете получить документ, полностью соответствующий оригиналу.
Превосходство этого решения состоит не только в том, что можно быстро получить свой диплом. Процесс организован удобно, с профессиональной поддержкой. От выбора подходящего образца до точного заполнения личных данных и доставки в любой регион России — все будет находиться под полным контролем квалифицированных специалистов.
Для тех, кто ищет быстрый способ получения требуемого документа, наша компания предлагает выгодное решение. Заказать диплом – это значит избежать долгого обучения и сразу переходить к достижению личных целей, будь то поступление в университет или начало профессиональной карьеры.
https://maps.google.com.mm/url?sa=t&url=https://rudiplomista.com
http://maps.google.com.ly/url?q=https://lands-diploma.com
https://cse.google.rw/url?sa=t&url=https://premialnie-diplomik.com
https://www.google.co.mz/url?q=https://premialnie-diplomik.com
https://www.google.sr/url?q=https://premialnie-diplomik.com
В современном мире, где диплом – это начало удачной карьеры в любом направлении, многие пытаются найти максимально быстрый путь получения образования. Наличие документа об образовании сложно переоценить. Ведь именно он открывает двери перед любым человеком, который стремится вступить в профессиональное сообщество или учиться в университете.
Наша компания предлагает максимально быстро получить этот необходимый документ. Вы сможете купить диплом, и это будет отличным решением для человека, который не смог закончить обучение, утратил документ или хочет исправить плохие оценки. диплом изготавливается аккуратно, с максимальным вниманием ко всем деталям, чтобы на выходе получился документ, полностью соответствующий оригиналу.
Преимущество такого решения заключается не только в том, что вы сможете оперативно получить диплом. Процесс организован комфортно, с профессиональной поддержкой. Начиная от выбора необходимого образца до правильного заполнения личных данных и доставки по России — все под полным контролем опытных специалистов.
Для тех, кто ищет оперативный способ получения требуемого документа, наша компания может предложить выгодное решение. Купить диплом – значит избежать продолжительного обучения и сразу переходить к своим целям: к поступлению в ВУЗ или к началу удачной карьеры.
https://diploman-rossiya.com
В нашем обществе, где диплом является началом отличной карьеры в любом направлении, многие ищут максимально быстрый и простой путь получения образования. Важность наличия официального документа об образовании трудно переоценить. Ведь именно диплом открывает двери перед всеми, кто собирается вступить в профессиональное сообщество или учиться в университете.
Предлагаем очень быстро получить любой необходимый документ. Вы имеете возможность заказать диплом, и это будет выгодным решением для всех, кто не смог закончить обучение или утратил документ. Все дипломы изготавливаются с особой аккуратностью, вниманием к мельчайшим нюансам. На выходе вы получите продукт, 100% соответствующий оригиналу.
Преимущество данного подхода заключается не только в том, что можно оперативно получить диплом. Процесс организован комфортно, с профессиональной поддержкой. От выбора подходящего образца до консультаций по заполнению личных данных и доставки по России — все будет находиться под абсолютным контролем опытных специалистов.
Для тех, кто ищет максимально быстрый способ получения требуемого документа, наша компания готова предложить отличное решение. Заказать диплом – значит избежать длительного процесса обучения и сразу переходить к личным целям, будь то поступление в университет или старт трудовой карьеры.
https://diploman-russiyan.com
В нашем обществе, где диплом – это начало удачной карьеры в любом направлении, многие пытаются найти максимально быстрый путь получения качественного образования. Наличие официального документа об образовании переоценить попросту невозможно. Ведь именно диплом открывает дверь перед любым человеком, который собирается вступить в сообщество квалифицированных специалистов или продолжить обучение в университете.
В данном контексте мы предлагаем максимально быстро получить этот необходимый документ. Вы сможете заказать диплом, и это становится отличным решением для всех, кто не смог завершить образование, утратил документ или желает исправить свои оценки. Каждый диплом изготавливается с особой аккуратностью, вниманием к мельчайшим нюансам, чтобы на выходе получился документ, 100% соответствующий оригиналу.
Плюсы подобного решения состоят не только в том, что можно максимально быстро получить диплом. Процесс организован просто и легко, с профессиональной поддержкой. Начиная от выбора необходимого образца диплома до консультаций по заполнению личной информации и доставки по России — все будет находиться под полным контролем качественных мастеров.
В результате, для тех, кто пытается найти быстрый способ получения необходимого документа, наша услуга предлагает выгодное решение. Заказать диплом – это значит избежать продолжительного обучения и не теряя времени перейти к достижению личных целей, будь то поступление в ВУЗ или начало удачной карьеры.
https://diploman-russiyan.com
FobertStand
Добрый день!
Диплом стал кошмаром, когда я отложил его выполнение и перешел на ночной график.
Приобретайте диплом университета без предоплаты у нас с доставкой в любой город России, гарантированное качество и безопасность.
Желаю всем честных отметок!
купить диплом в кисловодске
купить диплом колледжа
купить диплом в камышине
купить диплом в заречном
купить диплом в ессентуках
https://cse.google.ee/url?sa=t&url=https://kdiplom.ru/
https://maps.google.gg/url?q=https://kupite-diplom0024.ru/
https://www.google.com.om/url?sa=t&url=https://bisness-diplom.ru/
https://images.google.com.ar/url?sa=t&url=https://diplom5.com/
http://maps.google.cg/url?q=https://diplom-insti.ru/
В нашем мире, где диплом становится началом отличной карьеры в любом направлении, многие пытаются найти максимально быстрый путь получения качественного образования. Наличие документа об образовании переоценить попросту невозможно. Ведь диплом открывает дверь перед каждым человеком, который хочет начать профессиональную деятельность или учиться в каком-либо университете.
В данном контексте мы предлагаем оперативно получить этот необходимый документ. Вы можете купить диплом нового или старого образца, и это становится выгодным решением для всех, кто не смог завершить образование или утратил документ. Каждый диплом изготавливается с особой аккуратностью, вниманием к мельчайшим деталям. В результате вы сможете получить 100% оригинальный документ.
Превосходство такого решения заключается не только в том, что вы сможете быстро получить свой диплом. Весь процесс организован комфортно и легко, с профессиональной поддержкой. Начиная от выбора подходящего образца документа до консультаций по заполнению персональной информации и доставки по России — все будет находиться под абсолютным контролем качественных мастеров.
Всем, кто ищет быстрый и простой способ получения необходимого документа, наша компания предлагает выгодное решение. Приобрести диплом – значит избежать продолжительного обучения и сразу перейти к личным целям: к поступлению в ВУЗ или к началу трудовой карьеры.
https://www.google.at/url?q=https://rudiplomista.com
http://toolbarqueries.google.fr/url?sa=t&url=https://rudiplomista.com
https://www.google.co.zw/url?sa=t&url=https://lands-diploma.com
https://images.google.co.bw/url?sa=t&url=https://lands-diploma.com
https://images.google.be/url?q=https://rudiplomista.com
Admiring the time and energy you put into your website and in depth information you provide. It’s awesome to come across a blog every once in a while that isn’t the same outdated rehashed information. Great read! I’ve bookmarked your site and I’m adding your RSS feeds to my Google account.
https://www.google.ca/url?q=https://diplom5.com/
https://maps.google.gy/url?sa=j&url=https://nsk-diplom.com/
https://images.google.gy/url?q=https://diplom-profi.ru/
https://clients1.google.com.kw/url?sa=t&url=https://kupit-diplomyz24.com/
https://maps.google.com.sa/url?q=https://okdiplom.com/
В современном мире, где диплом является началом удачной карьеры в любом направлении, многие ищут максимально быстрый и простой путь получения качественного образования. Факт наличия документа об образовании трудно переоценить. Ведь диплом открывает двери перед всеми, кто собирается вступить в сообщество квалифицированных специалистов или учиться в ВУЗе.
Мы предлагаем быстро получить этот важный документ. Вы имеете возможность купить диплом нового или старого образца, что становится выгодным решением для всех, кто не смог завершить образование, утратил документ или желает исправить плохие оценки. Все дипломы изготавливаются с особой аккуратностью, вниманием ко всем нюансам, чтобы на выходе получился 100% оригинальный документ.
Превосходство такого решения состоит не только в том, что вы сможете быстро получить свой диплом. Весь процесс организовывается удобно, с профессиональной поддержкой. От выбора необходимого образца документа до консультации по заполнению личных данных и доставки по России — все будет находиться под абсолютным контролем качественных мастеров.
Для тех, кто хочет найти оперативный способ получить необходимый документ, наша компания предлагает выгодное решение. Купить диплом – значит избежать продолжительного процесса обучения и не теряя времени перейти к достижению собственных целей, будь то поступление в университет или старт карьеры.
https://diplomanc-russia24.com
OLaneAdoks
Добрый день!
Дипломное задание, казавшееся непреодолимым, стало легче благодаря интернет-ресурсам.
На нашем сайте вы можете купить диплом ВУЗа, недорого, с оплатой после получения, поддержка 24/7.
Желаю для каждого честных оценок!
купить диплом о среднем образовании
купить диплом менеджера по туризму
купить диплом в новочеркасске
купить диплом в иваново
купить диплом в ханты-мансийске
https://clients1.google.com.cu/url?sa=t&url=https://diplomoz-197.com/
https://cse.google.dj/url?sa=t&url=https://kupite-diplom0024.ru/
http://maps.google.iq/url?q=https://kazdiplomas.com/
https://cse.google.ms/url?sa=t&url=https://nsk-diplom.com/
https://cse.google.com.tr/url?q=https://diplomoz-197.com/
В нашем мире, где диплом становится началом удачной карьеры в любой сфере, многие ищут максимально быстрый и простой путь получения качественного образования. Важность наличия документа об образовании трудно переоценить. Ведь именно диплом открывает дверь перед людьми, стремящимися вступить в сообщество профессиональных специалистов или продолжить обучение в каком-либо институте.
В данном контексте мы предлагаем быстро получить этот важный документ. Вы имеете возможность купить диплом, что является отличным решением для всех, кто не смог закончить обучение или потерял документ. Все дипломы производятся аккуратно, с максимальным вниманием к мельчайшим элементам, чтобы в итоге получился полностью оригинальный документ.
Плюсы этого решения состоят не только в том, что вы сможете максимально быстро получить свой диплом. Весь процесс организован комфортно, с нашей поддержкой. От выбора требуемого образца до консультаций по заполнению личных данных и доставки в любое место страны — все под полным контролем качественных мастеров.
Всем, кто ищет оперативный способ получить требуемый документ, наша услуга предлагает выгодное решение. Купить диплом – значит избежать продолжительного процесса обучения и сразу переходить к своим целям, будь то поступление в ВУЗ или начало карьеры.
https://diploman-russiyans.com
В нашем мире, где диплом – это начало успешной карьеры в любом направлении, многие ищут максимально быстрый и простой путь получения качественного образования. Факт наличия документа об образовании переоценить невозможно. Ведь именно он открывает дверь перед любым человеком, который желает начать профессиональную деятельность или учиться в ВУЗе.
В данном контексте мы предлагаем оперативно получить этот важный документ. Вы можете купить диплом, что становится выгодным решением для человека, который не смог завершить образование, потерял документ или желает исправить свои оценки. Каждый диплом изготавливается аккуратно, с особым вниманием ко всем нюансам. В итоге вы сможете получить 100% оригинальный документ.
Плюсы данного подхода заключаются не только в том, что вы быстро получите диплом. Весь процесс организовывается удобно, с нашей поддержкой. От выбора требуемого образца до консультаций по заполнению персональной информации и доставки в любое место страны — все под абсолютным контролем наших мастеров.
Всем, кто пытается найти быстрый способ получить требуемый документ, наша услуга предлагает выгодное решение. Приобрести диплом – значит избежать длительного процесса обучения и не теряя времени перейти к достижению личных целей, будь то поступление в университет или начало карьеры.
https://diplomanc-russia24.com
В современном мире, где диплом становится началом успешной карьеры в любом направлении, многие ищут максимально быстрый путь получения образования. Факт наличия официального документа об образовании переоценить попросту невозможно. Ведь диплом открывает дверь перед каждым человеком, желающим вступить в профессиональное сообщество или продолжить обучение в ВУЗе.
Наша компания предлагает очень быстро получить любой необходимый документ. Вы можете заказать диплом старого или нового образца, что будет отличным решением для человека, который не смог закончить обучение или утратил документ. Любой диплом изготавливается с особой тщательностью, вниманием к мельчайшим элементам, чтобы в итоге получился документ, максимально соответствующий оригиналу.
Преимущество этого решения состоит не только в том, что можно оперативно получить диплом. Весь процесс организовывается удобно, с профессиональной поддержкой. Начав от выбора нужного образца документа до консультации по заполнению личных данных и доставки по России — все под абсолютным контролем качественных мастеров.
В результате, всем, кто хочет найти быстрый и простой способ получения необходимого документа, наша услуга предлагает выгодное решение. Заказать диплом – значит избежать длительного процесса обучения и не теряя времени перейти к своим целям, будь то поступление в университет или начало карьеры.
https://clients1.google.nl/url?sa=t&url=https://premialnie-diplomik.com
http://maps.google.pt/url?rct=j&sa=t&url=https://lands-diploma.com
https://www.google.co.bw/url?q=https://rudiplomista.com
https://www.google.co.vi/url?q=https://lands-diploma.com
http://cse.google.co.zw/url?sa=t&url=https://rudiplomista.com
Hello! Do you know if they make any plugins to help with SEO? I’m trying to get my blog to rank for some targeted keywords but I’m not seeing very good results. If you know of any please share. Many thanks!
https://clients1.google.com.kw/url?sa=t&url=https://peoplediplom.ru/
https://clients1.google.co.zm/url?q=https://kupit-diplomyz24.com/
https://cse.google.gy/url?sa=t&url=https://diplom-profi.ru/
https://toolbarqueries.google.cf/url?q=https://diplom-insti.ru/
https://cse.google.nr/url?sa=t&url=https://diploms-vuza.com/
На сегодняшний день, когда диплом – это начало удачной карьеры в любой сфере, многие ищут максимально быстрый путь получения качественного образования. Факт наличия документа об образовании трудно переоценить. Ведь диплом открывает двери перед людьми, желающими начать профессиональную деятельность или продолжить обучение в университете.
Наша компания предлагает оперативно получить любой необходимый документ. Вы имеете возможность купить диплом старого или нового образца, что становится выгодным решением для всех, кто не смог закончить обучение или утратил документ. Любой диплом изготавливается аккуратно, с особым вниманием к мельчайшим деталям. На выходе вы сможете получить полностью оригинальный документ.
Плюсы такого решения заключаются не только в том, что можно быстро получить диплом. Процесс организовывается удобно и легко, с профессиональной поддержкой. От выбора требуемого образца до точного заполнения персональной информации и доставки в любой регион страны — все под абсолютным контролем качественных мастеров.
В результате, для всех, кто ищет быстрый способ получить требуемый документ, наша компания предлагает отличное решение. Купить диплом – это значит избежать длительного процесса обучения и не теряя времени переходить к достижению личных целей: к поступлению в университет или к началу успешной карьеры.
https://diploman-russiyan.com
IsmaelLaw
Всем хорошего дня!
Диплом требует от меня изучения найденных в интернете материалов для улучшения качества работы.
Заказывайте диплом у нас и получите его быстро и безопасно, оплата по факту доставки, отправка в любой регион России.
Желаю всем пятерочных) оценок!
купить диплом в кропоткине
купить диплом повара
купить диплом в калининграде
купить диплом в красноярске
купить диплом во всеволожске
https://cse.google.co.ao/url?q=https://10000diplomov.ru/
http://maps.google.kz/url?q=https://prodiplome.com/
https://www.google.co.nz/url?sa=t&url=https://ry-diplom.com/
https://www.google.am/url?sa=t&url=https://diplom-zakaz.ru/
https://toolbarqueries.google.mn/url?q=https://diplom-zakaz.ru/
В нашем обществе, где диплом является началом удачной карьеры в любой области, многие пытаются найти максимально быстрый и простой путь получения образования. Необходимость наличия официального документа об образовании переоценить попросту невозможно. Ведь диплом открывает двери перед каждым человеком, желающим начать профессиональную деятельность или учиться в ВУЗе.
В данном контексте наша компания предлагает оперативно получить этот необходимый документ. Вы имеете возможность купить диплом, что является выгодным решением для человека, который не смог закончить образование, утратил документ или хочет исправить свои оценки. Каждый диплом изготавливается аккуратно, с максимальным вниманием к мельчайшим элементам. В результате вы сможете получить документ, максимально соответствующий оригиналу.
Превосходство такого решения состоит не только в том, что можно быстро получить диплом. Весь процесс организовывается комфортно, с профессиональной поддержкой. Начав от выбора необходимого образца диплома до консультации по заполнению персональной информации и доставки по стране — все находится под абсолютным контролем опытных специалистов.
Для всех, кто ищет быстрый и простой способ получить требуемый документ, наша компания предлагает отличное решение. Приобрести диплом – это значит избежать длительного процесса обучения и не теряя времени переходить к важным целям, будь то поступление в университет или начало карьеры.
https://diplomanc-russia24.com
В нашем обществе, где диплом становится началом успешной карьеры в любом направлении, многие ищут максимально быстрый и простой путь получения качественного образования. Важность наличия официального документа сложно переоценить. Ведь именно он открывает двери перед любым человеком, желающим вступить в профессиональное сообщество или продолжить обучение в университете.
Мы предлагаем оперативно получить этот важный документ. Вы можете купить диплом, что становится удачным решением для человека, который не смог завершить образование или потерял документ. Любой диплом изготавливается с особой аккуратностью, вниманием ко всем нюансам. В результате вы получите 100% оригинальный документ.
Преимущество такого решения состоит не только в том, что вы сможете быстро получить диплом. Процесс организован удобно, с нашей поддержкой. От выбора подходящего образца диплома до консультаций по заполнению личной информации и доставки в любой регион России — все под полным контролем квалифицированных специалистов.
Таким образом, всем, кто хочет найти максимально быстрый способ получить необходимый документ, наша компания предлагает выгодное решение. Заказать диплом – это значит избежать долгого обучения и сразу перейти к важным целям: к поступлению в ВУЗ или к началу трудовой карьеры.
https://diploman-russiyan.com
Сегодня, когда диплом является началом отличной карьеры в любой сфере, многие пытаются найти максимально быстрый путь получения качественного образования. Факт наличия официального документа об образовании трудно переоценить. Ведь именно диплом открывает двери перед каждым человеком, который стремится начать трудовую деятельность или учиться в высшем учебном заведении.
В данном контексте наша компания предлагает максимально быстро получить любой необходимый документ. Вы можете приобрести диплом, и это является выгодным решением для человека, который не смог завершить образование, потерял документ или желает исправить свои оценки. Все дипломы изготавливаются с особой тщательностью, вниманием ко всем деталям. В результате вы сможете получить документ, максимально соответствующий оригиналу.
Превосходство данного решения заключается не только в том, что вы быстро получите диплом. Весь процесс организовывается удобно, с профессиональной поддержкой. От выбора нужного образца документа до правильного заполнения личных данных и доставки в любое место страны — все под абсолютным контролем качественных мастеров.
Для всех, кто хочет найти максимально быстрый способ получить требуемый документ, наша компания предлагает выгодное решение. Купить диплом – значит избежать продолжительного процесса обучения и сразу перейти к достижению своих целей: к поступлению в университет или к началу успешной карьеры.
https://cse.google.sh/url?sa=t&url=https://rudiplomista.com
https://www.google.co.cr/url?q=https://lands-diploma.com
https://www.google.com.eg/url?q=https://premialnie-diplomik.com
http://maps.google.ro/url?q=https://lands-diploma.com
http://maps.google.ht/url?rct=j&sa=t&url=https://premialnie-diplomik.com
Здравствуйте!
Закажите российский диплом у нас по доступной цене с гарантией прохождения проверок и доставкой по РФ.
https://maps.google.com.pg/url?rct=j&sa=t&url=http://diplomsagroups.com
https://clients1.google.com.pa/url?sa=t&url=https://diplomansy.com
https://maps.google.com.mt/url?sa=t&url=https://eonline-diploms.com
https://maps.google.com.ua/url?q=https://russian-diplom.com
http://www.google.ms/url?sa=t&url=https://gosznac-diploma.com
Заказывайте диплом любого Вуза России у нас на сайте конфиденциально и без предоплаты.
FobertStand
Доброго дня!
Диплом теперь продвигается благодаря обширным онлайн-материалам.
Закажите диплом у нас – легко! Без предоплаты, с гарантией качества и доставкой по всей России.
Желаю всем положительных оценок!
купить свидетельство о заключении брака
купить диплом строителя
купить диплом в кинешме
купить диплом в оренбурге
купить диплом в каменске-шахтинском
https://toolbarqueries.google.mn/url?q=https://diplom-zakaz.ru/
https://maps.google.com.tr/url?q=https://diplom45.ru/
https://image.google.gl/url?q=https://10000diplomov.ru/
http://images.google.az/url?q=https://diplom-insti.ru/
http://toolbarqueries.google.co.in/url?sa=t&url=https://ry-diplom.com/
В нашем мире, где диплом становится началом успешной карьеры в любой отрасли, многие ищут максимально простой путь получения образования. Наличие официального документа трудно переоценить. Ведь диплом открывает дверь перед всеми, кто стремится начать профессиональную деятельность или продолжить обучение в ВУЗе.
Мы предлагаем максимально быстро получить этот важный документ. Вы имеете возможность приобрести диплом старого или нового образца, что становится отличным решением для человека, который не смог закончить обучение или потерял документ. дипломы изготавливаются с особой аккуратностью, вниманием ко всем деталям, чтобы в результате получился продукт, максимально соответствующий оригиналу.
Превосходство данного решения состоит не только в том, что можно оперативно получить диплом. Весь процесс организовывается комфортно, с нашей поддержкой. Начиная от выбора нужного образца диплома до грамотного заполнения личной информации и доставки по стране — все под полным контролем качественных специалистов.
Всем, кто хочет найти максимально быстрый способ получения необходимого документа, наша компания предлагает выгодное решение. Заказать диплом – значит избежать продолжительного обучения и сразу перейти к своим целям: к поступлению в ВУЗ или к началу удачной карьеры.
https://images.google.bg/url?q=https://rudiplomista.com
https://images.google.al/url?sa=t&url=https://rudiplomista.com
https://images.google.com.vn/url?sa=t&url=https://lands-diploma.com
http://maps.google.pt/url?rct=j&sa=t&url=https://premialnie-diplomik.com
https://maps.google.bg/url?sa=i&source=web&rct=j&url=https://premialnie-diplomik.com
Привет, дорогой читатель!
Получите диплом ВУЗа по выгодной цене с доставкой в любой город России без предоплаты и с гарантированной законностью документа!
https://cse.google.com.af/url?sa=t&url=https://gosznac-diploma.com
https://www.google.com.uy/url?q=https://anny-diploms.com
https://cse.google.off.ai/url?q=https://anny-diploms.com
https://cse.google.lv/url?q=https://anny-diploms.com
https://images.google.co.th/url?q=https://gosznac-diploma.com
Закажите диплом ВУЗа с доставкой по всей России без предоплаты и с гарантией качества!
Здравствуйте!
Закажите диплом ВУЗа недорого с доставкой курьером по России без предоплаты – это быстро и надежно!
https://www.google.fi/url?q=https://diplomansy.com
http://images.google.dm/url?q=https://eonline-diploms.com
https://images.google.gy/url?q=http://rdiplomik24.com
http://images.google.lk/url?sa=t&url=http://diploms-service.com
https://clients1.google.co.je/url?q=http://diplomrussian.com
Мы рады предложить вам приобрести диплом университета России по выгодной цене с доставкой в руки.
Lewiskneew
Добрый день!
Несмотря на все препятствия в работе над дипломом, я продолжаю находить способы его оптимизации благодаря интернету.
Закажите диплом в России без предоплаты и получите его с доставкой “под ключ”.
Желаю каждому не двоешных) отметок!
купить диплом в копейске
купить диплом в биробиджане
купить диплом в первоуральске
купить диплом в невинномысске
купить диплом в нижнем новгороде
http://maps.google.dm/url?q=https://prodiplome.com/
https://images.google.co.ma/url?q=https://diplomoz-197.com/
http://images.google.com.do/url?q=https://diplom-zakaz.ru/
https://images.google.co.ke/url?sa=t&url=https://peoplediplom.ru/
http://maps.google.cg/url?q=https://diplom-insti.ru/
Привет, дорогой читатель!
Приобретите диплом ВУЗа с гарантированной доставкой по России и без предварительной оплаты – надежно и выгодно!
https://maps.google.li/url?q=http://diplomsagroups.com
http://images.google.td/url?q=http://diplomsagroups.com
https://www.google.com.np/url?sa=t&url=http://originality-diplomy.com
https://www.google.com/url?sa=t&url=https://anny-diploms.com
https://ditu.google.com/url?q=http://diplomy-originaly.com
Наша компания предлагает широкий выбор дипломов Вузов России с доставкой по всей стране и гарантией качества.
Привет всем!
Получите российский диплом с гарантированной доставкой в любую точку страны без предварительной оплаты – просто и надежно!
http://maps.google.hr/url?q=https://diploms-asx.com
https://www.google.com.iq/url?sa=t&url=http://russdiplomiki.com
https://toolbarqueries.google.mn/url?q=https://premialnie-diplomansy.com
https://maps.google.co.zm/url?sa=j&rct=j&url=http://aurus-diploms.com
http://maps.google.kz/url?q=http://aurus-diploms.com
Наша компания поможет вам купить диплом ВУЗа с гарантией качества и доставкой в любой регион России!
Добрый день всем!
Получите российский диплом по доступной цене с гарантией прохождения проверок и доставкой в любой город РФ без предоплаты.
https://cse.google.sm/url?q=http://diplomy-originaly.com
http://images.google.co.nz/url?sa=t&url=http://originality-diplomy.com
https://www.google.com.tj/url?sa=t&url=http://free-diplommi.com
http://maps.google.vg/url?q=http://diplomsagroups.com
https://maps.google.co.mz/url?q=https://eonline-diploms.com
У нас вы можете заказать документы об образовании всех ВУЗов России с доставкой по РФ и оплатой после получения – просто и удобно!
В нашем обществе, где диплом – это начало успешной карьеры в любой отрасли, многие ищут максимально простой путь получения образования. Наличие документа об образовании сложно переоценить. Ведь именно диплом открывает дверь перед всеми, кто собирается вступить в сообщество профессиональных специалистов или продолжить обучение в ВУЗе.
Наша компания предлагает очень быстро получить этот необходимый документ. Вы сможете купить диплом старого или нового образца, что будет отличным решением для человека, который не смог завершить образование, потерял документ или хочет исправить плохие оценки. Любой диплом изготавливается с особой тщательностью, вниманием ко всем элементам. В результате вы получите продукт, 100% соответствующий оригиналу.
Преимущество такого решения состоит не только в том, что можно оперативно получить свой диплом. Процесс организовывается комфортно, с профессиональной поддержкой. От выбора необходимого образца до точного заполнения персональной информации и доставки в любое место страны — все будет находиться под абсолютным контролем качественных мастеров.
Всем, кто пытается найти быстрый способ получения необходимого документа, наша компания предлагает выгодное решение. Приобрести диплом – значит избежать длительного обучения и не теряя времени переходить к своим целям, будь то поступление в ВУЗ или начало профессиональной карьеры.
https://www.google.ie/url?q=https://russdiplomik.com
http://images.google.co.zm/url?q=https://russdiplomik.com
https://maps.google.com.au/url?q=https://gosznac-diplomy.com
http://cse.google.com.my/url?sa=t&url=https://gosznac-diplomy.com
https://maps.google.cm/url?q=https://originality-diplomiki.com
Lewiskneew
Приветики, дорогие мои!!
Подготовка диплома стала более продуктивной благодаря онлайн-ресурсам.
У нас можно заказать диплом без предоплаты с доставкой курьером по РФ, “под ключ”!
Желаю для каждого положительных оценок!
купить диплом в азове
купить диплом в ревде
купить диплом электрика
купить диплом в абакане
купить диплом для иностранцев
https://images.google.com.uy/url?q=https://diplom5.com/
https://cse.google.com.mx/url?q=https://kupite-diplom0024.ru/
https://www.google.at/url?q=https://kdiplom.ru/
http://cse.google.com.nf/url?sa=i&url=https://diploms-vuza.com/
https://cse.google.li/url?q=https://diplom5.com/
В современном мире, где диплом – это начало успешной карьеры в любом направлении, многие пытаются найти максимально быстрый путь получения качественного образования. Важность наличия официального документа об образовании трудно переоценить. Ведь именно диплом открывает двери перед людьми, стремящимися вступить в сообщество профессионалов или продолжить обучение в ВУЗе.
Предлагаем оперативно получить этот необходимый документ. Вы можете купить диплом, и это будет отличным решением для всех, кто не смог завершить образование, утратил документ или хочет исправить плохие оценки. Все дипломы изготавливаются с особой аккуратностью, вниманием ко всем деталям, чтобы в итоге получился 100% оригинальный документ.
Превосходство этого подхода заключается не только в том, что можно оперативно получить свой диплом. Весь процесс организовывается комфортно, с профессиональной поддержкой. От выбора требуемого образца документа до правильного заполнения личных данных и доставки в любой регион страны — все находится под полным контролем качественных мастеров.
В итоге, для тех, кто хочет найти быстрый и простой способ получить необходимый документ, наша компания предлагает отличное решение. Заказать диплом – это значит избежать продолжительного процесса обучения и не теряя времени переходить к своим целям: к поступлению в университет или к началу трудовой карьеры.
https://www.google.com.ua/url?q=https://originality-diplomiki.com
http://images.google.li/url?q=https://originality-diploman.com
https://cse.google.gl/url?sa=t&url=https://premialnie-diplomany.com
https://cse.google.com.co/url?sa=i&url=http://diploman-spb24.com
https://www.google.hu/url?q=http://rudiplomisty24.com
В современном мире, где диплом – это начало отличной карьеры в любом направлении, многие ищут максимально быстрый путь получения образования. Наличие официального документа об образовании трудно переоценить. Ведь диплом открывает двери перед каждым человеком, который хочет начать трудовую деятельность или учиться в университете.
В данном контексте мы предлагаем очень быстро получить этот важный документ. Вы сможете приобрести диплом нового или старого образца, и это становится отличным решением для всех, кто не смог завершить образование, потерял документ или хочет исправить свои оценки. дипломы изготавливаются аккуратно, с особым вниманием к мельчайшим элементам, чтобы в результате получился продукт, максимально соответствующий оригиналу.
Преимущество подобного подхода заключается не только в том, что можно максимально быстро получить диплом. Весь процесс организован комфортно, с профессиональной поддержкой. Начав от выбора требуемого образца до правильного заполнения личных данных и доставки в любое место страны — все будет находиться под абсолютным контролем качественных мастеров.
Всем, кто хочет найти оперативный способ получить необходимый документ, наша компания предлагает выгодное решение. Купить диплом – это значит избежать длительного процесса обучения и не теряя времени перейти к своим целям: к поступлению в ВУЗ или к началу трудовой карьеры.
https://cse.google.co.in/url?q=https://russdiplomik.com
https://maps.google.lk/url?sa=t&url=https://premialnie-diplomany.com
https://clients1.google.co.im/url?sa=t&url=http://volga-diplomy.com
http://images.google.com.na/url?q=http://volga-diplomy.com
http://images.google.co.nz/url?sa=t&url=https://premialnie-diplomany.com
В нашем мире, где диплом – это начало удачной карьеры в любой области, многие ищут максимально быстрый и простой путь получения качественного образования. Наличие официального документа об образовании трудно переоценить. Ведь диплом открывает двери перед каждым человеком, который желает вступить в профессиональное сообщество или продолжить обучение в ВУЗе.
Мы предлагаем максимально быстро получить этот важный документ. Вы имеете возможность приобрести диплом нового или старого образца, и это становится выгодным решением для всех, кто не смог завершить образование или потерял документ. Любой диплом изготавливается с особой тщательностью, вниманием ко всем элементам, чтобы в результате получился документ, полностью соответствующий оригиналу.
Преимущество такого решения состоит не только в том, что можно максимально быстро получить диплом. Процесс организован удобно и легко, с нашей поддержкой. Начиная от выбора требуемого образца документа до консультаций по заполнению личных данных и доставки по России — все под полным контролем опытных мастеров.
Таким образом, всем, кто пытается найти оперативный способ получить необходимый документ, наша компания предлагает выгодное решение. Приобрести диплом – значит избежать продолжительного процесса обучения и не теряя времени перейти к достижению своих целей: к поступлению в университет или к началу успешной карьеры.
https://clients1.google.com.cy/url?sa=t&url=https://russiany-diplomans.com
https://cse.google.vg/url?sa=t&url=http://rudiplomisty24.com
https://www.google.sc/url?q=https://lands-diploms.com
https://maps.google.la/url?q=https://premialnie-diplomany.com
https://maps.google.com.pg/url?rct=j&sa=t&url=http://rudiplomisty24.com
Dichaelvox
Всем хорошего дня!
Диплом стал моим кошмаром после перехода на ночные сессии работы.
Закажите диплом у нас и получите его быстро и надежно, оплатив после получения, с доставкой в любой регион РФ.
Желаю вам всем отличных оценок!
купить диплом оценщика
купить диплом в муроме
купить диплом геодезиста
купить диплом университета
купить диплом в костроме
https://images.google.co.mz/url?q=https://diplom5.com/
https://maps.google.co.id/url?sa=t&url=https://diplomoz-197.com/
http://images.google.com.na/url?q=https://prodiplome.com/
http://maps.google.so/url?q=https://kupite-diplom0024.ru/
http://alt1.toolbarqueries.google.co.ve/url?q=https://diplom5.com/
Приветики!
Получите документ ВУЗа без предоплаты и доставку в руки по России – просто, удобно, безопасно!
Хотите купить диплом Вуза недорого и получить его почтой без предоплаты? Мы можем помочь вам сделать это.
https://images.google.kg/url?q=http://rudiplomisty24.com
http://images.google.com.gh/url?sa=t&url=http://kazdiplom.com
https://www.google.co.uz/url?q=https://russiany-diplomans.com
https://clients1.google.rs/url?q=https://russdiplomag.com
http://maps.google.nl/url?q=https://rudiplomisty.com
В наше время, когда диплом – это начало успешной карьеры в любом направлении, многие стараются найти максимально быстрый путь получения качественного образования. Наличие документа об образовании сложно переоценить. Ведь диплом открывает двери перед людьми, стремящимися вступить в профессиональное сообщество или учиться в университете.
Предлагаем очень быстро получить этот важный документ. Вы имеете возможность заказать диплом нового или старого образца, и это становится выгодным решением для человека, который не смог закончить обучение или утратил документ. Любой диплом изготавливается с особой аккуратностью, вниманием к мельчайшим элементам, чтобы в итоге получился 100% оригинальный документ.
Преимущества такого решения состоят не только в том, что можно оперативно получить свой диплом. Процесс организован комфортно, с нашей поддержкой. От выбора необходимого образца до правильного заполнения персональной информации и доставки по России — все под абсолютным контролем квалифицированных специалистов.
Для всех, кто ищет максимально быстрый способ получения требуемого документа, наша компания предлагает выгодное решение. Приобрести диплом – значит избежать долгого обучения и не теряя времени перейти к своим целям, будь то поступление в ВУЗ или старт карьеры.
https://maps.google.dk/url?q=https://premialnie-diplomansy.com
https://cse.google.ws/url?sa=t&url=https://diploms-originalniy.com
http://cse.google.bt/url?sa=t&url=http://kazdiplom.com
https://cse.google.com.mt/url?q=https://originality-diplomiki.com
http://www.google.gr/url?q=https://originality-diploman.com
Привет, дорогой читатель!
Купите диплом ВУЗа по выгодной цене с гарантией качества и доставкой в любой город России без предоплаты – просто и надежно!
Получите диплом ВУЗа по выгодной цене с доставкой в любой город России без предоплаты и с гарантированной законностью документа!
https://images.google.co.za/url?q=https://gosznac-diplomy.com
https://www.google.cm/url?sa=i&rct=j&q=https://diploms-originalniy.com
https://cse.google.fi/url?sa=t&url=https://russdiplomag.com
https://www.google.at/url?q=https://russiany-diplomans.com
http://images.google.td/url?q=https://russdiplomag.com
В нашем мире, где диплом – это начало успешной карьеры в любом направлении, многие пытаются найти максимально быстрый и простой путь получения образования. Необходимость наличия документа об образовании переоценить невозможно. Ведь диплом открывает дверь перед каждым человеком, который хочет вступить в профессиональное сообщество или продолжить обучение в ВУЗе.
В данном контексте наша компания предлагает быстро получить этот необходимый документ. Вы сможете купить диплом старого или нового образца, что является отличным решением для всех, кто не смог завершить обучение, утратил документ или желает исправить свои оценки. диплом изготавливается с особой аккуратностью, вниманием ко всем нюансам, чтобы на выходе получился 100% оригинальный документ.
Плюсы подобного подхода заключаются не только в том, что можно оперативно получить диплом. Процесс организовывается комфортно, с профессиональной поддержкой. От выбора нужного образца документа до консультации по заполнению персональной информации и доставки по стране — все будет находиться под абсолютным контролем наших специалистов.
Для всех, кто пытается найти оперативный способ получения требуемого документа, наша компания предлагает выгодное решение. Заказать диплом – это значит избежать продолжительного обучения и сразу переходить к достижению собственных целей: к поступлению в университет или к началу трудовой карьеры.
http://www.google.cl/url?q=https://rudiplomisty.com
https://www.google.st/url?q=http://diploman-spb24.com
https://clients1.google.com.bn/url?sa=t&url=https://russdiplomag.com
https://clients1.google.com.ec/url?q=https://russiany-diplomans.com
https://www.google.de/url?q=https://russiany-diplomans.com
В современном мире, где диплом становится началом успешной карьеры в любой сфере, многие ищут максимально простой путь получения образования. Наличие документа об образовании переоценить просто невозможно. Ведь диплом открывает двери перед людьми, желающими вступить в профессиональное сообщество или продолжить обучение в высшем учебном заведении.
Мы предлагаем очень быстро получить любой необходимый документ. Вы имеете возможность заказать диплом старого или нового образца, и это будет отличным решением для всех, кто не смог закончить обучение или утратил документ. диплом изготавливается с особой тщательностью, вниманием ко всем деталям. В результате вы сможете получить 100% оригинальный документ.
Преимущества подобного подхода состоят не только в том, что можно оперативно получить диплом. Процесс организован комфортно, с профессиональной поддержкой. Начиная от выбора необходимого образца документа до консультаций по заполнению персональных данных и доставки по стране — все находится под абсолютным контролем наших мастеров.
В итоге, для всех, кто ищет максимально быстрый способ получения требуемого документа, наша компания готова предложить выгодное решение. Приобрести диплом – это значит избежать продолжительного обучения и не теряя времени переходить к своим целям: к поступлению в университет или к началу удачной карьеры.
https://toolbarqueries.google.td/url?sa=j&source=web&rct=j&url=https://lands-diploma.com
https://maps.google.no/url?rct=t&sa=t&url=https://lands-diploma.com
https://images.google.com.lb/url?q=https://premialnie-diplomik.com
https://www.google.com.pk/url?q=https://premialnie-diplomik.com
https://images.google.co.uk/url?sa=t&url=https://lands-diploma.com
Приветики!
Закажите диплом ВУЗа без предоплаты и получите его с доставкой в руки по всей России – это просто и удобно!
Купите диплом Гознака с гарантированной подлинностью и доставкой по всей России без предоплаты – просто и безопасно!
http://alt1.toolbarqueries.google.co.ve/url?q=http://diploman-spb24.com
https://images.google.com.eg/url?q=https://russdiplomag.com
http://posts.google.com/url?q=http://kazdiplom.com
https://images.google.com.pk/url?q=https://russdiplomag.com
http://maps.google.hn/url?rct=j&sa=t&url=https://originality-diplomiki.com
В нашем мире, где диплом – это начало отличной карьеры в любом направлении, многие ищут максимально быстрый и простой путь получения качественного образования. Факт наличия документа об образовании трудно переоценить. Ведь именно он открывает двери перед каждым человеком, который желает начать трудовую деятельность или учиться в любом институте.
Мы предлагаем очень быстро получить этот необходимый документ. Вы можете заказать диплом нового или старого образца, и это является выгодным решением для человека, который не смог закончить образование, утратил документ или хочет исправить плохие оценки. дипломы производятся с особой тщательностью, вниманием ко всем нюансам. В итоге вы получите документ, 100% соответствующий оригиналу.
Плюсы подобного подхода состоят не только в том, что вы максимально быстро получите диплом. Процесс организовывается комфортно, с нашей поддержкой. От выбора требуемого образца до консультации по заполнению персональных данных и доставки в любой регион страны — все находится под абсолютным контролем наших специалистов.
Всем, кто ищет оперативный способ получить необходимый документ, наша услуга предлагает выгодное решение. Купить диплом – значит избежать продолжительного процесса обучения и не теряя времени переходить к достижению собственных целей: к поступлению в университет или к началу трудовой карьеры.
https://maps.google.co.za/url?sa=t&url=https://premialnie-diplomansy.com
http://maps.google.ht/url?rct=j&sa=t&url=https://lands-diploms.com
http://www.google.mk/url?sa=i&url=https://gosznac-diplomy.com
https://www.google.co.ls/url?q=https://russdiplomik.com
https://maps.google.com.gh/url?sa=t&url=https://gosznac-diplomy.com
В современном мире, где диплом – это начало удачной карьеры в любой области, многие ищут максимально простой путь получения качественного образования. Необходимость наличия официального документа об образовании трудно переоценить. Ведь именно он открывает дверь перед всеми, кто собирается начать профессиональную деятельность или учиться в высшем учебном заведении.
В данном контексте мы предлагаем очень быстро получить этот важный документ. Вы сможете заказать диплом, что становится удачным решением для человека, который не смог завершить образование или потерял документ. дипломы производятся аккуратно, с максимальным вниманием ко всем деталям. В результате вы сможете получить 100% оригинальный документ.
Преимущество данного подхода состоит не только в том, что вы сможете максимально быстро получить диплом. Весь процесс организовывается удобно, с профессиональной поддержкой. От выбора подходящего образца до консультации по заполнению личной информации и доставки по стране — все будет находиться под абсолютным контролем квалифицированных специалистов.
В итоге, для всех, кто пытается найти быстрый и простой способ получить требуемый документ, наша компания готова предложить выгодное решение. Приобрести диплом – значит избежать долгого процесса обучения и сразу перейти к своим целям, будь то поступление в университет или начало карьеры.
https://images.google.com.gi/url?sa=t&url=http://diploman-spb24.com
https://maps.google.ki/url?sa=t&url=https://originality-diploman.com
https://www.google.com.om/url?sa=t&url=https://originality-diplomiki.com
https://maps.google.fi/url?q=http://rudiplomisty24.com
https://clients2.google.com/url?q=https://originality-diplomiki.com
В нашем обществе, где диплом – это начало успешной карьеры в любом направлении, многие стараются найти максимально простой путь получения качественного образования. Наличие документа об образовании трудно переоценить. Ведь диплом открывает дверь перед любым человеком, желающим вступить в профессиональное сообщество или продолжить обучение в университете.
В данном контексте мы предлагаем максимально быстро получить этот важный документ. Вы сможете купить диплом, что будет удачным решением для всех, кто не смог закончить обучение или утратил документ. дипломы производятся с особой аккуратностью, вниманием ко всем элементам. В итоге вы сможете получить 100% оригинальный документ.
Плюсы данного решения заключаются не только в том, что можно оперативно получить свой диплом. Весь процесс организовывается комфортно, с нашей поддержкой. От выбора подходящего образца до консультаций по заполнению личной информации и доставки в любое место России — все под полным контролем качественных специалистов.
Всем, кто ищет быстрый способ получения требуемого документа, наша компания может предложить отличное решение. Заказать диплом – это значит избежать продолжительного обучения и не теряя времени переходить к достижению своих целей: к поступлению в ВУЗ или к началу удачной карьеры.
http://maps.google.com.om/url?q=https://originality-diplomiki.com
https://images.google.com.my/url?q=http://rudiplomisty24.com
https://www.google.tm/url?sa=t&url=https://frees-diplom.com
https://www.google.com.ag/url?sa=t&url=https://premialnie-diplomansy.com
https://maps.google.co.bw/url?q=https://russdiplomag.com
В нашем обществе, где диплом является началом отличной карьеры в любом направлении, многие стараются найти максимально простой путь получения качественного образования. Необходимость наличия официального документа переоценить просто невозможно. Ведь диплом открывает дверь перед любым человеком, желающим вступить в сообщество профессиональных специалистов или учиться в каком-либо университете.
Мы предлагаем оперативно получить этот необходимый документ. Вы имеете возможность купить диплом, что становится выгодным решением для всех, кто не смог закончить обучение или потерял документ. Любой диплом изготавливается с особой аккуратностью, вниманием к мельчайшим элементам. На выходе вы получите 100% оригинальный документ.
Плюсы подобного решения заключаются не только в том, что можно оперативно получить свой диплом. Весь процесс организовывается удобно, с профессиональной поддержкой. Начав от выбора необходимого образца до консультации по заполнению персональных данных и доставки по стране — все под абсолютным контролем квалифицированных специалистов.
В результате, для тех, кто ищет быстрый способ получить необходимый документ, наша услуга предлагает отличное решение. Купить диплом – значит избежать продолжительного процесса обучения и сразу перейти к достижению личных целей, будь то поступление в ВУЗ или начало карьеры.
https://maps.google.com.au/url?q=https://frees-diplom.com
http://www.google.co.ao/url?q=https://russdiplomag.com
http://maps.google.kz/url?q=https://originality-diplomiki.com
https://maps.google.bt/url?sa=t&url=https://gosznac-diplomy.com
https://www.google.ba/url?sa=t&url=https://diploms-originalniy.com
В нашем мире, где диплом – это начало удачной карьеры в любом направлении, многие ищут максимально быстрый путь получения образования. Наличие официального документа сложно переоценить. Ведь диплом открывает двери перед людьми, стремящимися вступить в сообщество профессионалов или учиться в каком-либо университете.
В данном контексте наша компания предлагает оперативно получить этот важный документ. Вы сможете купить диплом нового или старого образца, и это становится отличным решением для человека, который не смог завершить образование или утратил документ. дипломы изготавливаются с особой аккуратностью, вниманием к мельчайшим нюансам, чтобы на выходе получился 100% оригинальный документ.
Превосходство этого подхода заключается не только в том, что вы сможете оперативно получить свой диплом. Весь процесс организовывается удобно, с профессиональной поддержкой. От выбора подходящего образца до грамотного заполнения личных данных и доставки в любое место России — все под полным контролем квалифицированных специалистов.
В результате, для тех, кто ищет быстрый и простой способ получить требуемый документ, наша услуга предлагает выгодное решение. Купить диплом – это значит избежать продолжительного обучения и сразу переходить к достижению собственных целей, будь то поступление в ВУЗ или начало успешной карьеры.
https://www.google.com.ai/url?q=https://frees-diplom.com
https://images.google.bi/url?q=http://rudiplomisty24.com
https://images.google.ee/url?sa=j&source=web&rct=j&url=https://russdiplomag.com
https://image.google.co.ck/url?sa=j&source=web&rct=j&url=https://frees-diplom.com
https://www.google.com.ec/url?q=https://frees-diplom.com
I think that everything wrote was very logical. However, consider this, suppose you were to create a awesome headline? I am not saying your information isn’t solid., but what if you added something that makes people want more? I mean %BLOG_TITLE% is kinda boring. You might peek at Yahoo’s front page and note how they write news titles to grab people to open the links. You might add a video or a picture or two to grab readers interested about what you’ve got to say. Just my opinion, it would bring your posts a little livelier.
https://controlc.com/7105d373
Hey there! Do you know if they make any plugins to protect against hackers? I’m kinda paranoid about losing everything I’ve worked hard on. Any recommendations?
https://postheaven.net/samirigica/remont-abo-zamina-korpusu-fari-iak-pravil-no-priiniati-rishennia
Сегодня, когда диплом – это начало отличной карьеры в любой отрасли, многие пытаются найти максимально быстрый и простой путь получения качественного образования. Факт наличия официального документа об образовании трудно переоценить. Ведь диплом открывает дверь перед людьми, желающими вступить в профессиональное сообщество или учиться в университете.
Наша компания предлагает максимально быстро получить любой необходимый документ. Вы сможете приобрести диплом, что становится отличным решением для всех, кто не смог завершить образование или утратил документ. Каждый диплом изготавливается аккуратно, с особым вниманием к мельчайшим нюансам, чтобы в результате получился 100% оригинальный документ.
Преимущества данного решения заключаются не только в том, что вы сможете быстро получить диплом. Весь процесс организован комфортно, с нашей поддержкой. От выбора требуемого образца до консультаций по заполнению личной информации и доставки по России — все под абсолютным контролем качественных специалистов.
Всем, кто ищет быстрый способ получить необходимый документ, наша компания готова предложить отличное решение. Приобрести диплом – это значит избежать долгого процесса обучения и сразу переходить к достижению личных целей, будь то поступление в университет или старт успешной карьеры.
https://cse.google.co.il/url?sa=t&url=http://volga-diplomy.com
https://cse.google.lv/url?q=http://volga-diplomy.com
https://images.google.co.za/url?q=https://lands-diploms.com
http://toolbarqueries.google.it/url?sa=t&url=https://russdiplomik.com
http://maps.google.ht/url?rct=j&sa=t&url=http://rudiplomisty24.com
Good day! This post couldn’t be written any better! Reading this post reminds me of my good old room mate! He always kept chatting about this. I will forward this page to him. Pretty sure he will have a good read. Thank you for sharing!
https://blogfreely.net/abbotsoutm/h1-b-kupiti-sklo-far-farfarlight-nadiinist-ta-stil-dlia-vashogo
В наше время, когда диплом – это начало успешной карьеры в любом направлении, многие ищут максимально быстрый и простой путь получения качественного образования. Важность наличия официального документа об образовании сложно переоценить. Ведь именно диплом открывает дверь перед каждым человеком, желающим начать трудовую деятельность или продолжить обучение в университете.
В данном контексте наша компания предлагает очень быстро получить этот необходимый документ. Вы можете купить диплом нового или старого образца, и это становится выгодным решением для человека, который не смог закончить обучение, утратил документ или хочет исправить плохие оценки. дипломы изготавливаются с особой аккуратностью, вниманием ко всем нюансам. В результате вы получите полностью оригинальный документ.
Плюсы данного решения заключаются не только в том, что можно быстро получить диплом. Процесс организовывается комфортно, с профессиональной поддержкой. Начиная от выбора необходимого образца диплома до правильного заполнения личной информации и доставки в любой регион страны — все находится под полным контролем качественных специалистов.
Для всех, кто пытается найти оперативный способ получить требуемый документ, наша компания готова предложить выгодное решение. Заказать диплом – значит избежать продолжительного обучения и сразу переходить к достижению собственных целей: к поступлению в ВУЗ или к началу трудовой карьеры.
https://groups.google.com/g/opencoweb-devhttp://rudiplomisty24.com
https://clients1.google.com.kw/url?sa=t&url=https://originality-diploman.com
http://www.google.gr/url?q=http://volga-diplomy.com
https://www.google.ge/url?q=https://originality-diplomiki.com
https://maps.google.bg/url?sa=i&source=web&rct=j&url=https://diploms-originalniy.com
В нашем мире, где диплом – это начало удачной карьеры в любой области, многие ищут максимально быстрый и простой путь получения образования. Наличие документа об образовании переоценить невозможно. Ведь диплом открывает двери перед каждым человеком, который хочет начать трудовую деятельность или учиться в высшем учебном заведении.
В данном контексте мы предлагаем максимально быстро получить этот необходимый документ. Вы сможете заказать диплом старого или нового образца, что будет отличным решением для человека, который не смог закончить образование, утратил документ или желает исправить плохие оценки. Каждый диплом изготавливается с особой аккуратностью, вниманием к мельчайшим нюансам. В итоге вы получите полностью оригинальный документ.
Плюсы подобного подхода состоят не только в том, что можно оперативно получить диплом. Весь процесс организовывается удобно, с нашей поддержкой. Начиная от выбора требуемого образца до грамотного заполнения личных данных и доставки по стране — все будет находиться под абсолютным контролем квалифицированных мастеров.
Всем, кто хочет найти быстрый и простой способ получения требуемого документа, наша компания готова предложить отличное решение. Заказать диплом – это значит избежать долгого обучения и не теряя времени переходить к достижению собственных целей, будь то поступление в университет или начало профессиональной карьеры.
https://cse.google.com.tw/url?q=http://volga-diplomy.com
http://images.google.com.bh/url?sa=t&url=http://volga-diplomy.com
http://www.google.by/url?q=http://diploman-spb24.com
http://www.google.sn/url?q=https://premialnie-diplomansy.com
https://cse.google.com.ec/url?sa=t&url=http://diploman-spb24.com
В нашем мире, где диплом – это начало отличной карьеры в любом направлении, многие ищут максимально быстрый путь получения образования. Наличие документа об образовании переоценить невозможно. Ведь диплом открывает двери перед любым человеком, желающим начать трудовую деятельность или учиться в каком-либо ВУЗе.
Наша компания предлагает оперативно получить этот необходимый документ. Вы можете заказать диплом, что будет удачным решением для всех, кто не смог закончить обучение или утратил документ. диплом изготавливается с особой аккуратностью, вниманием ко всем элементам, чтобы в итоге получился продукт, 100% соответствующий оригиналу.
Преимущества подобного решения заключаются не только в том, что вы сможете быстро получить диплом. Весь процесс организовывается комфортно и легко, с нашей поддержкой. От выбора требуемого образца документа до правильного заполнения персональных данных и доставки в любое место России — все находится под абсолютным контролем наших мастеров.
Всем, кто ищет оперативный способ получения необходимого документа, наша услуга предлагает выгодное решение. Заказать диплом – значит избежать длительного процесса обучения и не теряя времени перейти к важным целям, будь то поступление в ВУЗ или начало карьеры.
http://www.google.gr/url?q=http://rudiplomisty24.com
https://images.google.kg/url?q=https://premialnie-diplomany.com
https://clients1.google.com.bn/url?sa=t&url=https://diploms-originalniy.com
https://images.google.com.kw/url?q=https://premialnie-diplomany.com
https://clients1.google.mv/url?rct=j&sa=t&url=https://originality-diplomiki.com
В нашем обществе, где диплом – это начало удачной карьеры в любой области, многие ищут максимально быстрый и простой путь получения образования. Наличие документа об образовании сложно переоценить. Ведь диплом открывает дверь перед каждым человеком, который стремится вступить в профессиональное сообщество или продолжить обучение в ВУЗе.
Наша компания предлагает быстро получить этот важный документ. Вы имеете возможность заказать диплом нового или старого образца, что становится выгодным решением для всех, кто не смог закончить обучение или потерял документ. диплом изготавливается с особой тщательностью, вниманием к мельчайшим элементам. На выходе вы получите 100% оригинальный документ.
Превосходство этого решения заключается не только в том, что можно оперативно получить диплом. Весь процесс организован просто и легко, с нашей поддержкой. Начиная от выбора требуемого образца диплома до точного заполнения персональной информации и доставки в любое место страны — все под абсолютным контролем квалифицированных мастеров.
В итоге, для тех, кто ищет оперативный способ получения требуемого документа, наша услуга предлагает выгодное решение. Заказать диплом – значит избежать длительного процесса обучения и сразу перейти к достижению собственных целей: к поступлению в университет или к началу трудовой карьеры.
http://cse.google.bt/url?sa=t&url=https://premialnie-diplomany.com
http://alt1.toolbarqueries.google.com.gi/url?q=http://rudiplomisty24.com
https://www.google.mv/url?sa=t&url=https://originality-diplomiki.com
https://clients1.google.no/url?sa=t&url=https://russdiplomik.com
http://www.google.com.cy/url?q=http://rudiplomisty24.com
Сегодня, когда диплом является началом удачной карьеры в любой области, многие пытаются найти максимально быстрый и простой путь получения качественного образования. Наличие официального документа об образовании сложно переоценить. Ведь именно он открывает дверь перед людьми, стремящимися начать трудовую деятельность или учиться в высшем учебном заведении.
В данном контексте наша компания предлагает оперативно получить этот необходимый документ. Вы имеете возможность купить диплом, и это будет выгодным решением для всех, кто не смог завершить образование, потерял документ или хочет исправить свои оценки. диплом изготавливается с особой аккуратностью, вниманием ко всем деталям. В результате вы получите 100% оригинальный документ.
Преимущества данного решения состоят не только в том, что можно максимально быстро получить свой диплом. Весь процесс организовывается комфортно, с нашей поддержкой. Начав от выбора нужного образца документа до правильного заполнения персональных данных и доставки в любой регион страны — все под абсолютным контролем квалифицированных специалистов.
В итоге, для тех, кто пытается найти оперативный способ получения требуемого документа, наша компания готова предложить выгодное решение. Заказать диплом – значит избежать долгого обучения и сразу перейти к своим целям: к поступлению в ВУЗ или к началу удачной карьеры.
https://cse.google.sc/url?sa=t&url=https://originality-diploman.com
https://clients1.google.lv/url?sa=t&url=http://kazdiplom.com
https://www.google.com.ua/url?q=http://rudiplomisty24.com
https://www.google.com.sv/url?sa=t&url=https://premialnie-diplomansy.com
http://maps.google.vg/url?q=http://volga-diplomy.com
В нашем обществе, где диплом становится началом удачной карьеры в любом направлении, многие стараются найти максимально быстрый и простой путь получения образования. Наличие документа об образовании переоценить невозможно. Ведь именно диплом открывает двери перед всеми, кто стремится начать трудовую деятельность или учиться в университете.
Наша компания предлагает оперативно получить этот важный документ. Вы можете приобрести диплом старого или нового образца, что будет отличным решением для всех, кто не смог завершить образование или утратил документ. дипломы производятся аккуратно, с особым вниманием ко всем элементам, чтобы на выходе получился продукт, 100% соответствующий оригиналу.
Преимущества данного решения состоят не только в том, что можно быстро получить диплом. Весь процесс организован комфортно, с профессиональной поддержкой. От выбора нужного образца документа до консультации по заполнению личной информации и доставки по России — все под полным контролем квалифицированных мастеров.
Всем, кто ищет быстрый способ получить необходимый документ, наша компания готова предложить отличное решение. Приобрести диплом – это значит избежать длительного обучения и не теряя времени перейти к достижению собственных целей: к поступлению в ВУЗ или к началу успешной карьеры.
diploman-russia.com
Купить диплом с переводом на английский
купить диплом [url=http://www.diplom-msk.ru]http://www.diplom-msk.ru[/url] .
В нашем обществе, где диплом – это начало отличной карьеры в любой сфере, многие ищут максимально быстрый путь получения качественного образования. Необходимость наличия официального документа трудно переоценить. Ведь именно он открывает дверь перед каждым человеком, желающим вступить в профессиональное сообщество или продолжить обучение в любом ВУЗе.
В данном контексте наша компания предлагает оперативно получить этот необходимый документ. Вы сможете приобрести диплом старого или нового образца, и это является отличным решением для человека, который не смог закончить обучение или потерял документ. диплом изготавливается аккуратно, с максимальным вниманием ко всем нюансам, чтобы в итоге получился полностью оригинальный документ.
Преимущества этого подхода заключаются не только в том, что можно оперативно получить диплом. Весь процесс организован комфортно, с профессиональной поддержкой. От выбора подходящего образца до консультаций по заполнению личных данных и доставки по России — все будет находиться под абсолютным контролем опытных специалистов.
В итоге, для тех, кто ищет быстрый способ получить требуемый документ, наша услуга предлагает отличное решение. Приобрести диплом – это значит избежать долгого процесса обучения и не теряя времени перейти к важным целям: к поступлению в университет или к началу трудовой карьеры.
http://www.diploman-russiyan.com
Сегодня, когда диплом является началом успешной карьеры в любом направлении, многие пытаются найти максимально быстрый путь получения качественного образования. Наличие официального документа об образовании переоценить просто невозможно. Ведь именно он открывает двери перед людьми, стремящимися начать профессиональную деятельность или учиться в каком-либо ВУЗе.
В данном контексте наша компания предлагает оперативно получить этот необходимый документ. Вы можете купить диплом, что является выгодным решением для всех, кто не смог закончить обучение или утратил документ. дипломы производятся аккуратно, с максимальным вниманием ко всем нюансам, чтобы в итоге получился документ, полностью соответствующий оригиналу.
Преимущество этого подхода заключается не только в том, что можно быстро получить свой диплом. Процесс организовывается просто и легко, с нашей поддержкой. Начав от выбора необходимого образца до консультации по заполнению персональной информации и доставки по России — все находится под абсолютным контролем опытных мастеров.
Таким образом, для всех, кто ищет быстрый способ получить необходимый документ, наша компания предлагает выгодное решение. Заказать диплом – значит избежать продолжительного процесса обучения и не теряя времени перейти к важным целям: к поступлению в ВУЗ или к началу трудовой карьеры.
http://www.diploman-russiyan.com
Привет, дорогой читатель!
Купите диплом ВУЗа с гарантированной доставкой в любой город России без предварительной оплаты и уверенностью в его легальности!
Наша компания поможет купить диплом Вуза со скидкой и доставкой в любую точку России
https://clients1.google.com.tr/url?sa=t&url=https://premialnie-diplomany.com
http://images.google.je/url?q=https://russdiplomik.com
https://maps.google.at/url?q=http://diploman-spb24.com
https://images.google.al/url?sa=t&url=http://volga-diplomy.com
https://clients1.google.com.bd/url?q=https://russdiplomag.com
Привет всем!
На нашем сайте вы можете заказать диплом ВУЗа недорого с возможностью оплаты после получения и круглосуточной поддержкой!
На нашем сайте вы можете заказать диплом ВУЗа недорого с возможностью оплаты после получения и круглосуточной поддержкой!
https://www.google.com.mt/url?sa=t&url=https://frees-diplom.com
https://clients1.google.lv/url?sa=t&url=https://russiany-diplomans.com
http://images.google.com.tj/url?q=https://rudiplomisty.com
https://image.google.am/url?q=http://volga-diplomy.com
https://clients1.google.no/url?sa=t&url=https://originality-diplomiki.com
В современном мире, где диплом – это начало успешной карьеры в любом направлении, многие ищут максимально быстрый и простой путь получения качественного образования. Наличие документа об образовании переоценить попросту невозможно. Ведь диплом открывает двери перед каждым человеком, который хочет вступить в сообщество профессионалов или учиться в высшем учебном заведении.
Мы предлагаем очень быстро получить любой необходимый документ. Вы сможете заказать диплом, что будет удачным решением для человека, который не смог закончить обучение или утратил документ. Все дипломы производятся с особой аккуратностью, вниманием ко всем нюансам, чтобы в результате получился 100% оригинальный документ.
Преимущество этого подхода заключается не только в том, что вы быстро получите диплом. Весь процесс организовывается удобно, с нашей поддержкой. Начав от выбора необходимого образца диплома до грамотного заполнения персональной информации и доставки по России — все под полным контролем наших мастеров.
Всем, кто ищет быстрый способ получить требуемый документ, наша компания предлагает выгодное решение. Приобрести диплом – значит избежать долгого процесса обучения и не теряя времени перейти к достижению своих целей: к поступлению в ВУЗ или к началу успешной карьеры.
vuzdiploma
В нашем обществе, где диплом является началом успешной карьеры в любой отрасли, многие ищут максимально простой путь получения образования. Наличие официального документа об образовании переоценить просто невозможно. Ведь именно он открывает дверь перед каждым человеком, который собирается вступить в сообщество профессиональных специалистов или продолжить обучение в каком-либо ВУЗе.
Наша компания предлагает очень быстро получить этот важный документ. Вы имеете возможность заказать диплом, и это будет выгодным решением для всех, кто не смог закончить обучение, утратил документ или желает исправить плохие оценки. Все дипломы производятся с особой аккуратностью, вниманием ко всем элементам, чтобы на выходе получился документ, максимально соответствующий оригиналу.
Плюсы этого решения заключаются не только в том, что можно оперативно получить свой диплом. Весь процесс организовывается удобно, с нашей поддержкой. От выбора нужного образца документа до правильного заполнения личных данных и доставки в любой регион России — все будет находиться под полным контролем наших мастеров.
Для всех, кто ищет быстрый способ получить требуемый документ, наша компания предлагает выгодное решение. Приобрести диплом – значит избежать продолжительного процесса обучения и сразу переходить к достижению собственных целей, будь то поступление в университет или старт профессиональной карьеры.
http://diplomvam.ru
Доброго всем дня!
Закажите диплом ВУЗа с доставкой по России без предоплаты и с возможностью оплаты после получения – надежно, выгодно, безопасно!
Приобретите российский диплом по выгодной цене с гарантией проверки и доставкой в любой город РФ – без предоплаты!
https://asia.google.com/url?q=https://gosznac-diplomy.com
https://www.google.co.ma/url?sa=t&url=https://originality-diplomiki.com
https://clients2.google.com/url?q=https://originality-diplomiki.com
http://cse.google.com.gt/url?sa=t&url=https://premialnie-diplomansy.com
http://toolbarqueries.google.it/url?sa=t&url=https://originality-diplomiki.com
Hi excellent website! Does running a blog like this require a massive amount work? I’ve very little understanding of coding however I was hoping to start my own blog in the near future. Anyhow, if you have any ideas or tips for new blog owners please share. I know this is off topic however I simply had to ask. Thanks a lot!
https://animedia.xyz/
В нашем мире, где диплом является началом удачной карьеры в любом направлении, многие ищут максимально простой путь получения образования. Факт наличия официального документа об образовании трудно переоценить. Ведь именно он открывает двери перед каждым человеком, желающим начать трудовую деятельность или учиться в высшем учебном заведении.
Наша компания предлагает оперативно получить этот необходимый документ. Вы имеете возможность купить диплом, что становится удачным решением для всех, кто не смог закончить обучение или потерял документ. диплом изготавливается аккуратно, с особым вниманием к мельчайшим элементам. В результате вы сможете получить продукт, максимально соответствующий оригиналу.
Превосходство этого решения состоит не только в том, что вы сможете максимально быстро получить диплом. Процесс организовывается комфортно и легко, с профессиональной поддержкой. От выбора подходящего образца документа до правильного заполнения персональной информации и доставки по стране — все находится под абсолютным контролем качественных мастеров.
Таким образом, всем, кто ищет максимально быстрый способ получения требуемого документа, наша компания готова предложить выгодное решение. Купить диплом – это значит избежать длительного обучения и не теряя времени переходить к личным целям, будь то поступление в университет или старт трудовой карьеры.
http://www.vsediplomu.ru
В современном мире, где диплом – это начало успешной карьеры в любом направлении, многие ищут максимально простой путь получения образования. Наличие официального документа об образовании сложно переоценить. Ведь именно диплом открывает дверь перед людьми, стремящимися вступить в сообщество профессиональных специалистов или учиться в ВУЗе.
В данном контексте мы предлагаем оперативно получить этот важный документ. Вы имеете возможность купить диплом старого или нового образца, и это становится отличным решением для человека, который не смог завершить образование, потерял документ или желает исправить свои оценки. диплом изготавливается аккуратно, с особым вниманием ко всем нюансам. В результате вы получите документ, полностью соответствующий оригиналу.
Преимущество этого решения состоит не только в том, что можно быстро получить диплом. Весь процесс организован комфортно, с нашей поддержкой. От выбора необходимого образца до правильного заполнения личной информации и доставки в любое место страны — все находится под полным контролем наших мастеров.
В итоге, всем, кто ищет быстрый и простой способ получения требуемого документа, наша компания готова предложить отличное решение. Приобрести диплом – это значит избежать длительного процесса обучения и сразу перейти к достижению собственных целей, будь то поступление в университет или начало карьеры.
http://www.diplomany.ru
В нашем мире, где диплом – это начало успешной карьеры в любом направлении, многие стараются найти максимально быстрый и простой путь получения качественного образования. Наличие официального документа об образовании трудно переоценить. Ведь именно диплом открывает двери перед каждым человеком, который желает начать профессиональную деятельность или учиться в ВУЗе.
В данном контексте мы предлагаем оперативно получить этот важный документ. Вы сможете заказать диплом, и это становится отличным решением для всех, кто не смог завершить образование или потерял документ. диплом изготавливается с особой аккуратностью, вниманием к мельчайшим элементам. В результате вы сможете получить 100% оригинальный документ.
Плюсы подобного решения состоят не только в том, что вы максимально быстро получите диплом. Процесс организовывается просто и легко, с профессиональной поддержкой. От выбора требуемого образца документа до консультаций по заполнению личных данных и доставки в любое место страны — все будет находиться под абсолютным контролем наших мастеров.
В результате, для тех, кто ищет быстрый и простой способ получить требуемый документ, наша компания предлагает отличное решение. Приобрести диплом – значит избежать продолжительного обучения и не теряя времени переходить к достижению личных целей: к поступлению в университет или к началу удачной карьеры.
https://www.google.co.mz/url?q=https://originality-diplomiki.com
https://maps.google.cl/url?q=https://russdiplomag.com
https://cse.google.lu/url?q=https://rudiplomisty.com
https://cse.google.com.ua/url?q=http://kazdiplom.com
https://www.google.com.cu/url?q=http://diploman-spb24.com
Сегодня, когда диплом становится началом успешной карьеры в любой отрасли, многие ищут максимально простой путь получения качественного образования. Наличие официального документа об образовании переоценить невозможно. Ведь диплом открывает дверь перед любым человеком, желающим вступить в профессиональное сообщество или учиться в каком-либо университете.
Наша компания предлагает оперативно получить этот необходимый документ. Вы имеете возможность заказать диплом, что будет выгодным решением для всех, кто не смог закончить образование, утратил документ или хочет исправить плохие оценки. Любой диплом изготавливается аккуратно, с максимальным вниманием ко всем нюансам, чтобы в итоге получился полностью оригинальный документ.
Преимущества этого решения состоят не только в том, что можно оперативно получить диплом. Процесс организован комфортно и легко, с нашей поддержкой. От выбора требуемого образца до правильного заполнения личных данных и доставки в любой регион страны — все находится под абсолютным контролем опытных специалистов.
В итоге, для тех, кто ищет быстрый и простой способ получить требуемый документ, наша компания предлагает отличное решение. Заказать диплом – значит избежать продолжительного обучения и не теряя времени перейти к важным целям, будь то поступление в ВУЗ или старт карьеры.
http://99diplomov.ru
В современном мире, где диплом становится началом удачной карьеры в любой отрасли, многие ищут максимально быстрый путь получения качественного образования. Наличие официального документа переоценить просто невозможно. Ведь именно он открывает дверь перед любым человеком, который хочет вступить в профессиональное сообщество или продолжить обучение в университете.
В данном контексте мы предлагаем быстро получить этот необходимый документ. Вы можете купить диплом, что будет отличным решением для всех, кто не смог закончить обучение, утратил документ или хочет исправить плохие оценки. Любой диплом изготавливается аккуратно, с особым вниманием к мельчайшим деталям. В итоге вы сможете получить продукт, полностью соответствующий оригиналу.
Превосходство подобного подхода заключается не только в том, что вы сможете оперативно получить диплом. Весь процесс организован комфортно, с профессиональной поддержкой. От выбора необходимого образца до правильного заполнения персональной информации и доставки по стране — все будет находиться под полным контролем наших специалистов.
В итоге, для тех, кто пытается найти оперативный способ получения необходимого документа, наша услуга предлагает отличное решение. Купить диплом – это значит избежать длительного обучения и сразу переходить к своим целям: к поступлению в ВУЗ или к началу успешной карьеры.
http://www.ab-diplom.ru
В современном мире, где диплом – это начало отличной карьеры в любой отрасли, многие ищут максимально простой путь получения образования. Необходимость наличия официального документа об образовании переоценить просто невозможно. Ведь диплом открывает дверь перед любым человеком, который собирается начать трудовую деятельность или учиться в высшем учебном заведении.
Мы предлагаем очень быстро получить этот важный документ. Вы имеете возможность приобрести диплом, что становится выгодным решением для человека, который не смог завершить обучение, утратил документ или желает исправить свои оценки. дипломы производятся с особой аккуратностью, вниманием к мельчайшим деталям, чтобы на выходе получился полностью оригинальный документ.
Превосходство подобного решения заключается не только в том, что можно максимально быстро получить свой диплом. Весь процесс организован комфортно, с профессиональной поддержкой. Начав от выбора нужного образца документа до консультации по заполнению персональных данных и доставки в любое место страны — все под полным контролем качественных специалистов.
В итоге, для тех, кто ищет оперативный способ получения необходимого документа, наша компания может предложить выгодное решение. Заказать диплом – значит избежать долгого процесса обучения и не теряя времени переходить к своим целям: к поступлению в ВУЗ или к началу трудовой карьеры.
diplom-msk.ru
В нашем мире, где диплом становится началом удачной карьеры в любой сфере, многие ищут максимально быстрый и простой путь получения образования. Наличие официального документа об образовании сложно переоценить. Ведь именно диплом открывает двери перед каждым человеком, желающим вступить в сообщество профессионалов или учиться в высшем учебном заведении.
В данном контексте мы предлагаем очень быстро получить этот важный документ. Вы можете купить диплом, что будет отличным решением для человека, который не смог закончить образование, утратил документ или хочет исправить свои оценки. дипломы производятся с особой аккуратностью, вниманием ко всем нюансам, чтобы в итоге получился документ, максимально соответствующий оригиналу.
Преимущества этого подхода состоят не только в том, что вы сможете оперативно получить свой диплом. Весь процесс организовывается удобно, с нашей поддержкой. Начав от выбора нужного образца диплома до консультации по заполнению персональной информации и доставки по стране — все будет находиться под полным контролем опытных мастеров.
Для тех, кто ищет быстрый и простой способ получить требуемый документ, наша услуга предлагает выгодное решение. Заказать диплом – значит избежать долгого процесса обучения и сразу перейти к достижению собственных целей, будь то поступление в ВУЗ или старт удачной карьеры.
http://www.diplom-gotovie.ru
Hi there Dear, are you actually visiting this website on a regular basis, if so then you will without doubt get fastidious know-how.
http://diplom07.ru
Because the admin of this web site is working, no question very quickly it will be famous, due to its feature contents.
http://www.server-attestats.com
В нашем обществе, где диплом является началом удачной карьеры в любом направлении, многие ищут максимально быстрый путь получения качественного образования. Наличие официального документа переоценить просто невозможно. Ведь диплом открывает двери перед людьми, стремящимися начать профессиональную деятельность или продолжить обучение в ВУЗе.
Мы предлагаем максимально быстро получить любой необходимый документ. Вы имеете возможность купить диплом нового или старого образца, и это является выгодным решением для человека, который не смог закончить обучение или утратил документ. Все дипломы изготавливаются аккуратно, с особым вниманием к мельчайшим нюансам, чтобы в результате получился продукт, максимально соответствующий оригиналу.
Превосходство данного подхода состоит не только в том, что вы сможете максимально быстро получить диплом. Весь процесс организован просто и легко, с профессиональной поддержкой. Начав от выбора необходимого образца до консультации по заполнению персональных данных и доставки по России — все находится под абсолютным контролем квалифицированных мастеров.
В итоге, всем, кто пытается найти быстрый способ получения необходимого документа, наша компания предлагает отличное решение. Купить диплом – значит избежать долгого процесса обучения и сразу перейти к достижению личных целей: к поступлению в университет или к началу удачной карьеры.
man-attestats24.com
В современном мире, где диплом является началом успешной карьеры в любой сфере, многие ищут максимально быстрый путь получения качественного образования. Необходимость наличия официального документа переоценить невозможно. Ведь диплом открывает дверь перед всеми, кто собирается вступить в профессиональное сообщество или продолжить обучение в ВУЗе.
В данном контексте мы предлагаем очень быстро получить этот важный документ. Вы можете купить диплом, и это будет выгодным решением для всех, кто не смог завершить образование или потерял документ. диплом изготавливается с особой аккуратностью, вниманием к мельчайшим нюансам. В итоге вы сможете получить 100% оригинальный документ.
Преимущество данного решения состоит не только в том, что можно оперативно получить диплом. Процесс организовывается удобно, с профессиональной поддержкой. Начав от выбора необходимого образца до точного заполнения личной информации и доставки в любой регион России — все будет находиться под полным контролем качественных специалистов.
Всем, кто пытается найти оперативный способ получить необходимый документ, наша услуга предлагает отличное решение. Приобрести диплом – значит избежать длительного процесса обучения и сразу перейти к достижению собственных целей, будь то поступление в университет или начало карьеры.
https://vuzdiploma.ru /
Приветики!
Закажите диплом ВУЗа с гарантированной доставкой по России без предоплаты и с гарантией качества – просто и надежно!
Приобретите диплом института или колледжа недорого с доставкой по РФ и гарантией качества без предварительной оплаты!
http://images.google.co.uz/url?sa=t&url=https://originality-diploman.com
http://images.google.co.zm/url?q=https://russiany-diplomans.com
https://clients1.google.com.sl/url?sa=t&url=https://premialnie-diplomany.com
https://image.google.am/url?q=https://rudiplomisty.com
https://www.google.com.tn/url?q=http://diploman-spb24.com
В нашем мире, где диплом становится началом отличной карьеры в любой сфере, многие ищут максимально быстрый и простой путь получения образования. Факт наличия документа об образовании переоценить невозможно. Ведь диплом открывает дверь перед всеми, кто желает начать трудовую деятельность или учиться в ВУЗе.
Мы предлагаем максимально быстро получить любой необходимый документ. Вы имеете возможность приобрести диплом, что является выгодным решением для человека, который не смог закончить обучение, потерял документ или желает исправить свои оценки. дипломы выпускаются аккуратно, с максимальным вниманием ко всем деталям, чтобы на выходе получился документ, полностью соответствующий оригиналу.
Преимущество данного решения заключается не только в том, что вы сможете оперативно получить диплом. Весь процесс организовывается комфортно, с профессиональной поддержкой. От выбора требуемого образца до консультаций по заполнению личных данных и доставки по стране — все под абсолютным контролем наших мастеров.
В итоге, для тех, кто хочет найти оперативный способ получения требуемого документа, наша компания может предложить отличное решение. Приобрести диплом – значит избежать продолжительного обучения и сразу перейти к достижению своих целей, будь то поступление в университет или старт успешной карьеры.
http://russa24-attestats.com
Сегодня, когда диплом – это начало удачной карьеры в любом направлении, многие ищут максимально простой путь получения образования. Факт наличия официального документа переоценить попросту невозможно. Ведь диплом открывает двери перед каждым человеком, который стремится начать профессиональную деятельность или продолжить обучение в ВУЗе.
Мы предлагаем очень быстро получить любой необходимый документ. Вы имеете возможность заказать диплом, и это будет удачным решением для всех, кто не смог завершить обучение, потерял документ или хочет исправить плохие оценки. диплом изготавливается с особой тщательностью, вниманием к мельчайшим элементам. На выходе вы получите документ, максимально соответствующий оригиналу.
Преимущество этого решения заключается не только в том, что можно максимально быстро получить диплом. Процесс организовывается комфортно, с профессиональной поддержкой. Начиная от выбора нужного образца до точного заполнения персональных данных и доставки по России — все под абсолютным контролем качественных специалистов.
Всем, кто ищет максимально быстрый способ получения необходимого документа, наша компания предлагает выгодное решение. Заказать диплом – это значит избежать долгого процесса обучения и сразу перейти к достижению собственных целей: к поступлению в университет или к началу трудовой карьеры.
http://www.saksx-attestats.ru
В нашем мире, где диплом является началом удачной карьеры в любом направлении, многие стараются найти максимально быстрый и простой путь получения образования. Факт наличия документа об образовании переоценить попросту невозможно. Ведь именно диплом открывает дверь перед всеми, кто стремится начать трудовую деятельность или продолжить обучение в высшем учебном заведении.
В данном контексте наша компания предлагает оперативно получить этот важный документ. Вы можете приобрести диплом, что является отличным решением для всех, кто не смог завершить образование или потерял документ. диплом изготавливается с особой аккуратностью, вниманием ко всем элементам, чтобы в итоге получился полностью оригинальный документ.
Преимущества такого подхода состоят не только в том, что можно оперативно получить диплом. Весь процесс организовывается удобно и легко, с нашей поддержкой. От выбора требуемого образца документа до консультаций по заполнению личных данных и доставки в любое место страны — все будет находиться под полным контролем качественных мастеров.
Таким образом, для тех, кто хочет найти максимально быстрый способ получить требуемый документ, наша компания может предложить отличное решение. Купить диплом – это значит избежать продолжительного процесса обучения и не теряя времени перейти к достижению собственных целей, будь то поступление в университет или начало успешной карьеры.
diploman-russia.ru
Купить Диплом Строительный
Единственное, что отличает документ, выданный в образовательном учреждении и полученный в нашей компании отсутствие в базе. У нас огромный опыт работы в сфере услуг по созданию дипломов, в день мы осуществляем более десятка заказов, на цену не влияет ни вуз, ни оценки, ни специальность. Преимуществ сотрудничества с нами много, начиная от доступной стоимости услуг, и заканчивая быстрыми дипломами Строительный выполнения каждого заказа. Обратитесь к профессионалам, и ваш новый диплом станет первой ступенью на пути к вершинам карьерных достижений Воспользуйтесь нашими возможностями, чтобы приблизить то будущее, о котором вы купили. Сам факт, что на руках присутствует красный диплом, уже многое значит, а что за всем этим стоит уже совсем ни кого не волнует.
http://www.russkiy365-diploms-srednee.ru
Купить Диплом О Высшем Образовании В Калининграде
Мы купимте за качественную услугу чуть больше, но отдаем вам товар практически по себестоимости. На сегодняшний день большой популярностью пользуется профессия провизора или фармацевта. В первую очередь, это связано с тем, что на территории России дипломы, выданные в Украине, Белоруссии и Казахстане действуют на уровне с выданными национальными ВУЗами, но отношение работодателей немного отличается и наличия степени магистр, является весомым преимуществом при приёме на работу. Через несколько лет вчерашние студенты, получив диплом, легко найдут работу себе по душе.
Купить Диплом Юриста С Занесением В Реестр
За несколько лет, которые придётся купить за партой университета ради формального диплома, можно достичь неплохих результатов, наработать нужный опыт, практические навыки. Во-первых, в образовании начинают использоваться инструменты обучения с применением ИТ онлайн-курсы, симуляторы, тренажеры, игровые онлайн-миры. Решение купить диплом Строительный о высшем образовании принимается в непредвиденных ситуациях.
Кандидат Наук
Не нужна защита диплома, квалификация подтверждается итоговой аттестацией. Текучка кадров в ней все ещё высока, но кандидатов на профессию менеджера турфирмы или гида достаточно. Как и университеты, колледжи бывают двух видов: училища гражданской авиации и военные авиационные училища. Нужно знать ответ на такой вопрос, как чем отличается академия от университета. Первая задача чемпионата – выявление, развитие и поддержка талантливой, перспективной молодежи молодых специалистов, обладающих высоким уровнем профессионального мастерства и содействие их трудоустройству.
russkiy365-diploms-srednee.ru
Диплом Бакалавра Купить
Общее охватывает дошкольное и школьное образование, а профессиональное – среднее и высшее. В подобных ситуациях мы предлагаем купить кандидат вуза, техникума, института или колледжа и остаться работать на прежнем месте. Магистр образовательный уровень специалистов, который по достоинству оценивается на рынке труда и открывает множество перспектив, но в то же время, требует дополнительной траты времени и финансов. Большинство людей решаются на такой шаг в следующих ситуациях: желание получить повышение на работе.
Свидетельство О Рождении 2009 Года
Вся информация должна быть актуальной на дату выдачи диплома, соответствовать нормативным требованиям и корректной. Воспользоваться первым кандидатом Наук, возможно, будет честнее, но на него необходимо потратить несколько лет. Восстановление займёт очень много времени и может оказаться сложно осуществимой задачей через множество причин.
Сколько Страниц В Дипломе 2017
Мы готовы предоставить на данный спрос качественное предложение. У нас все покупки конфиденциальные, а дипломы выполнены на таком уровне, что спокойно проходят проверки любого уровня. Завершение школьной учебы и получение диплома о среднем образовании являются ключевыми моментами в жизни каждого человека. Избежать таких страниц В Дипломе 2017 и следующих за ними проблем, можно путём своевременного оформления специального документа в паре со свидетельством о разводе. Мы подготовим дипломную, которая заслужит положительную оценку как научного руководителя и рецензента, так и в целом государственной аттестационной комиссии. Самое лучшее решение купить диплом бакалавра и решить проблему.
https://arusak-diploms-srednee.ru
Купить Диплом Университета
Про ФДО ТУСУР мне повезло услышать от студентов, уже закончивших этот факультет, после чего я стала целенаправленно искать информацию о нём в СМИ. Для покупки “корочки” не понадобится сдавать вступительные экзамены, тратить время на посещение лекций и сдачу экзаменов, зачетов, курсовых. Мы разработали абсолютно безопасный способ взаимодействия с клиентом: вы оставляете заявку на покупку диплома вуза, колледжа, техникума или пту, в течение 13 дней документы проходят подготовку и предварительную проверку, а затем передаются курьерской службе, после личного получения диплома вы тщательно осматриваете документ на предмет безошибочности заполнения и аутентичности бланков, все верно.
Нужно Ли Подтверждать Диплом Медсестры
Оставлять семью, бросать работу и отправится учиться, или же как все студенты-заочники, попросту оплачивать сессии. Мы предоставляем только качественный товар дипломы, удостоверения, справки, аттестаты, свидетельства и прочие документы, выполненные на оригинальных бланках ГоЗнак. Кроме этого, бакалавр это выпускник ВУЗа с полноценным высшим образованием.
Hi, its fastidious post about media print, we all be familiar with media is a fantastic source of facts.
http://seriallove.bbok.ru/viewtopic.php?id=6721#p122679
http://shkola6309.ru/forums/forum/vneurochnaya-deyatelnost/
http://ya.9bb.ru/viewtopic.php?id=5015#p10098
https://school97.ru/vesti/view_profile.php?UID=207540
http://kadastr.bestbb.ru/viewtopic.php?id=1198#p1985
Hi! Do you use Twitter? I’d like to follow you if that would be okay. I’m absolutely enjoying your blog and look forward to new posts.
http://politictoday.ru/preimushhestva-pokupki-diploma-put-k-luchshemu-budushhemu
https://iqtorg.ru/forum/messages/forum2/topic546/message604/?result=new#message604
http://polegasm.net/index.php/forum/welcome-mat/151192
http://wiki.gsksurvey.ru/пїЅпїЅпїЅпїЅпїЅ_пїЅ_пїЅпїЅпїЅ_пїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅ_пїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅ:_пїЅпїЅпїЅпїЅпїЅпїЅ_пїЅпїЅпїЅпїЅпїЅпїЅ_пїЅпїЅпїЅпїЅпїЅ_пїЅпїЅпїЅпїЅпїЅпїЅ
http://kolhos.listbb.ru/viewtopic.php?f=2&t=403
It’s remarkable for me to have a web site, which is useful for my know-how. thanks admin
http://realniemoney.0pk.me/viewtopic.php?id=4280#p9896
https://flowersfixprice.ru/forum/user/148620/
http://www.paladiny.ru/forummess.dwar.php?TopicID=27077
http://avrorp.getbb.ru/viewtopic.php?f=183&t=614
https://abris-zip.ru/company/personal/user/190/forum/edit/new/
Thank you for the auspicious writeup. It in fact was once a leisure account it. Look complicated to more added agreeable from you! However, how could we keep in touch?
http://anusnasiki.mybb.ru/viewtopic.php?id=451#p611
http://bestworld.getbb.ru/viewtopic.php?f=8&t=1099
http://kinogonews.ru/zakaz-dokumentov-o-prohozhdenii-kursov
http://censornet.ru/diplomyi-po-vashim-trebovaniyam-u-nas-est-to-chto-vam-nuzhno/
http://aboutalltour.ru/diplom-po-vashim-trebovaniyam-gde-zakazat-obrazovanie-bez-riskov/
I enjoy, cause I discovered just what I was taking a look for. You have ended my four day long hunt! God Bless you man. Have a great day. Bye
https://stav.goodbb.ru/viewtopic.php?id=10025#p27769
http://www.chaodisiaque.com/forum/viewtopic.php?pid=21855#p21855
http://www.mirmafii.ru/article/7240
http://eurodelo.ru/zakazat-diplom-legko-byistro-nadezhno
http://crimea.bestbb.ru/viewtopic.php?id=491#p624
Hey! I realize this is sort of off-topic but I had to ask. Does managing a well-established blog such as yours take a lot of work? I’m brand new to operating a blog but I do write in my journal on a daily basis. I’d like to start a blog so I can easily share my personal experience and views online. Please let me know if you have any ideas or tips for brand new aspiring bloggers. Thankyou!
https://www.benedeek.com/blogs/79468/пїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅ-пїЅпїЅпїЅпїЅпїЅпїЅ-пїЅ-пїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅ-пїЅпїЅпїЅпїЅпїЅпїЅ-пїЅпїЅпїЅ-пїЅпїЅпїЅпїЅпїЅпїЅ-пїЅпїЅпїЅпїЅпїЅпїЅ
http://pokemon-go.onl/users/6146
https://www.industrialagency.org/blogs/56143/пїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅ-пїЅпїЅпїЅпїЅпїЅ-пїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅ-пїЅпїЅ-пїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅ
http://visacart.80lvl.ru/viewtopic.php?f=1&t=660
https://prof-komplekt.com/club/user/4861/blog/9986/
I used to be able to find good info from your content.
http://pdlspd.listbb.ru/viewtopic.php?f=3&t=327
http://rodina.listbb.ru/viewtopic.php?f=3&t=407
http://jivonews.ru/kupit-diplom-vasha-vozmozhnost-byit-uspeshnyim-bez-lishnih-usiliy
http://g95334gq.beget.tech/2024/05/13/diplom-po-vashim-trebovaniyam-gde-zakazat-obrazovanie-s-vygodoy.html
https://prof-komplekt.com/club/user/4861/blog/9986/
Hey just wanted to give you a quick heads up and let you know a few of the pictures aren’t loading properly. I’m not sure why but I think its a linking issue. I’ve tried it in two different web browsers and both show the same outcome.
http://itbitgroup.ru/poluchite-diplom-prosto-byistro-nadezhno
http://forum.astrakhan.ru/gallery/image/1401-пїЅпїЅпїЅпїЅпїЅпїЅ-пїЅпїЅпїЅпїЅпїЅпїЅ-пїЅпїЅпїЅ-пїЅпїЅпїЅпїЅпїЅпїЅ-пїЅпїЅпїЅпїЅпїЅпїЅпїЅ-пїЅпїЅпїЅпїЅпїЅпїЅ-пїЅпїЅпїЅпїЅпїЅпїЅпїЅ-пїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅ/
http://forumkasino.bestff.ru/viewtopic.php?id=3705#p8732
http://darknews.ru/uspeh-bez-granits-kupit-diplom-i-raskryit-potentsial
http://diablomania.ru/forum/showthread.php?p=563274#post563274
I’m gone to tell my little brother, that he should also pay a quick visit this weblog on regular basis to get updated from most recent news update.
http://jivonews.ru/kupit-diplom-vasha-vozmozhnost-byit-uspeshnyim-bez-lishnih-usiliy
http://flashtest.80lvl.ru/viewtopic.php?f=3&t=1816
http://anotherfirstmagicwar.mybb.ru/viewtopic.php?id=342#p567
http://t98223u0.beget.tech/2024/04/27/diplom-vashey-mechty-my-pomozhem-vam-ego-dostich.html
http://1-click.pl/excelforum/viewtopic.php?f=3&t=162002
What’s up, all is going fine here and ofcourse every one is sharing information, that’s really good, keep up writing.
http://vsetutonline.com/forum/member.php?u=76509
https://www.danishwomenorg.com/read-blog/3102
https://www.4x4zubry.by/forum/messages/forum1/topic1586/message178067/?result=new#message178067
What a material of un-ambiguity and preserveness of valuable knowledge about unpredicted emotions.
http://www.matchfishing.ru/forumtest/1/member.php?u=23110
http://www.pets-ural.ru/content/forum/posting.php
https://asktourist.ru/viewtopic.php?id=4934#p18724
Hello to all, how is the whole thing, I think every one is getting more from this site, and your views are pleasant for new people.
http://aranzhirovki.ru/smf/index.php?topic=4222.0
http://art-gymnastics.ru/users/54
http://pokemon-go.onl/users/6146
Hi there to every one, it’s actually a nice for me to visit this site, it contains precious Information.
http://bohhchaos.listbb.ru/viewtopic.php?f=9&t=7833
https://ssa.ru/forum/kupit-diplom-vasha-dver-k-luchshemu-buduschemu-i-uspeshnoi-karere.html
http://ya.9bb.ru/viewtopic.php?id=5089#p10201
Can you tell us more about this? I’d want to find out some additional information.
https://nhlfriends.com/read-blog/3298
http://wow-tour.ru/diplom-po-vashemu-vyiboru-garantirovannoe-kachestvo-i-konfidentsialnost
http://startinvest.2bb.ru/viewtopic.php?id=10277#p53592
Wow, amazing blog format! How long have you ever been running a blog for? you made running a blog look easy. The entire look of your website is wonderful, as well as the content material!
https://mylady.mybb.ru/viewtopic.php?id=27875#p126142
http://3drus.ru/forum/topic_34716
http://www.tamboff.ru/forum/viewtopic.php?p=7696950#7696950
Attractive element of content. I just stumbled upon your website and in accession capital to claim that I get in fact loved account your weblog posts. Any way I will be subscribing on your augment or even I achievement you get right of entry to persistently quickly.
https://volnodumie.bbmy.ru/viewtopic.php?id=11777#p23897
http://finttech.ru/kupit-diplom-vasha-investitsiya-v-budushhee
http://www.odnopolchane.net/forum/member.php?u=546804
An impressive share! I’ve just forwarded this onto a coworker who had been doing a little homework on this. And he in fact bought me lunch due to the fact that I found it for him… lol. So allow me to reword this…. Thanks for the meal!! But yeah, thanx for spending time to discuss this matter here on your internet site.
https://www.ukwomenorg.com/read-blog/4711
https://safdfpb.ixbb.ru/viewtopic.php?id=14#p14
http://thelspr.listbb.ru/viewtopic.php?f=13&t=263
Thanks , I’ve just been looking for information about this subject for ages and yours is the greatest I have came upon so far. However, what about the conclusion? Are you sure in regards to the supply?
https://kharkov-balka.com/showthread.php?p=152590#post152590
https://visogo9427.ixbb.ru/viewtopic.php?id=12#p12
http://mybaltika.info/ru/blogs/587/9346/
Hello, I want to subscribe for this web site to obtain most up-to-date updates, therefore where can i do it please help out.
http://pgdvanho.edu.vn/index.php?language=vi&nv=statistics&nvvithemever=t&nv_redirect=aHR0cHM6Ly9hZGlzZ3J1bnRsZWRyZXB1YmxpY2FuLmNvbQ
http://psp1zdzieszowice.edu.pl/2017/09/21/narodowy-dzien-interpunkcji/
https://open.mit.edu/profile/01HY38MNMGT65YXW8RKHTG4AD6/
https://disqus.com/by/disqus_geBo5wnVd7/about/
https://gravatar.com/josearnold2
Hi it’s me, I am also visiting this web site on a regular basis, this website is in fact fastidious and the users are actually sharing nice thoughts.
https://bookmarkfavors.com/story2581790/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2%D0%BE%D0%BB%D0%B3%D0%BE%D0%B4%D0%BE%D0%BD%D1%81%D0%BA
http://moy-pitomec.ru/category/horses
https://pozdravit-vsex.ru/s-dnem-rozhdeniya/7-let/
http://oceanmining.ru/shop/473343
https://quadro-mebel.ru/
В нашем мире, где диплом – это начало отличной карьеры в любой сфере, многие ищут максимально быстрый и простой путь получения образования. Необходимость наличия официального документа об образовании переоценить попросту невозможно. Ведь именно диплом открывает двери перед каждым человеком, который стремится вступить в профессиональное сообщество или продолжить обучение в университете.
Мы предлагаем очень быстро получить этот важный документ. Вы можете купить диплом, и это является отличным решением для всех, кто не смог завершить образование или потерял документ. Каждый диплом изготавливается с особой аккуратностью, вниманием к мельчайшим нюансам. В результате вы сможете получить 100% оригинальный документ.
Плюсы такого решения состоят не только в том, что вы максимально быстро получите свой диплом. Процесс организовывается комфортно, с нашей поддержкой. Начав от выбора нужного образца документа до грамотного заполнения личной информации и доставки по России — все находится под полным контролем опытных специалистов.
Всем, кто хочет найти быстрый и простой способ получения необходимого документа, наша компания предлагает отличное решение. Купить диплом – значит избежать длительного обучения и не теряя времени переходить к своим целям: к поступлению в ВУЗ или к началу удачной карьеры.
http://www.diplomsagroups.com
Can you tell us more about this? I’d love to find out some additional information.
https://pro-cofe.ru/kofein-kofeynogo-dereva/
https://battlefield.ru/ivan-krutitsyn.html
https://bookmarkleader.com/story17145832/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%81%D0%BF%D0%B5%D1%86%D0%B8%D0%B0%D0%BB%D0%B8%D1%81%D1%82%D0%B0
https://zvezda-receptov.ru/?p=12241
https://www.agrimoto.fr/
Good day! This is my 1st comment here so I just wanted to give a quick shout out and say I really enjoy reading through your blog posts. Can you recommend any other blogs/websites/forums that cover the same topics? Thank you so much!
musey-uglich.ru
Можете выбрать грифы для гантелей на https://grify-dlya-gantely.ru/по недорогим ценамоптимальной длины. В выпуске долговечных изделий активно используются высококлассные марки металла. Грифы для гантелей создаются в трех популярных диаметрах. Снаряды разработаны для силовых занятий и созданы с разметкой для правильного размещения рук и рифлением для уверенного хвата. Изделия покрываются защитным слоем никеля. Отечественная компания предлагает широкий ассортимент спортивного инвентаря для квартиры и фитнес центра. Это универсальный инвентарь для силовых тренировок в любых условиях.