Angular Cheilitis: Symptoms & Treatment
An inflammatory illness called angular cheilitis results in red, puffy areas on the corners of the mouth. It is brought on by specific bacterial or fungal illnesses, and treatment usually works well. However, this is a typical inflammatory skin disorder. As a result, it is noticed by signs of inflamed, cracking sores on one or both corners of your mouth. Although uncomfortable, this condition typically doesn’t get worse.

Other names for angular cheilitis include perleche and angular stomatitis. The difference between cold sores and angular cheilitis are often confusing. However, cold sores are a distinct ailment that are pre signs of the herpes virus. Thus, this condition is not communicable, unlike cold sores.
Who is prone to this condition?
The extremely young and very old tend to be the groups most susceptible to this condition. As a result, elderly persons may have sagging skin at their mouth corners or wear dentures, which can contribute to dry mouth corners. On the other hand, infant mouths can become irritated by pacifiers, thumb sucking, and drooling.
What causes angular cheilitis?
Dryness is brought on by saliva accumulating at the corners of the mouth. Thus, this condition can develop in this location due to extremely dry skin. As a result, the dry skin may eventually start to break open. Sometimes fungi or bacteria find their way into the cracks, which can lead to infection or inflammation. The following factors can lead to dry, cracked lip corners and angular cheilitis:
- Eczema Or Atopic Dermatitis.
- Not Fitting Dentures.
- Drooling When You Sleep.
- Oral Infections Caused By Fungi Or Yeast, Such Thrush.
- Crooked Teeth.
- Skin Conditions.
- Using A Pacifier Or Thumb To Sucky.
- Masking One’s Face.
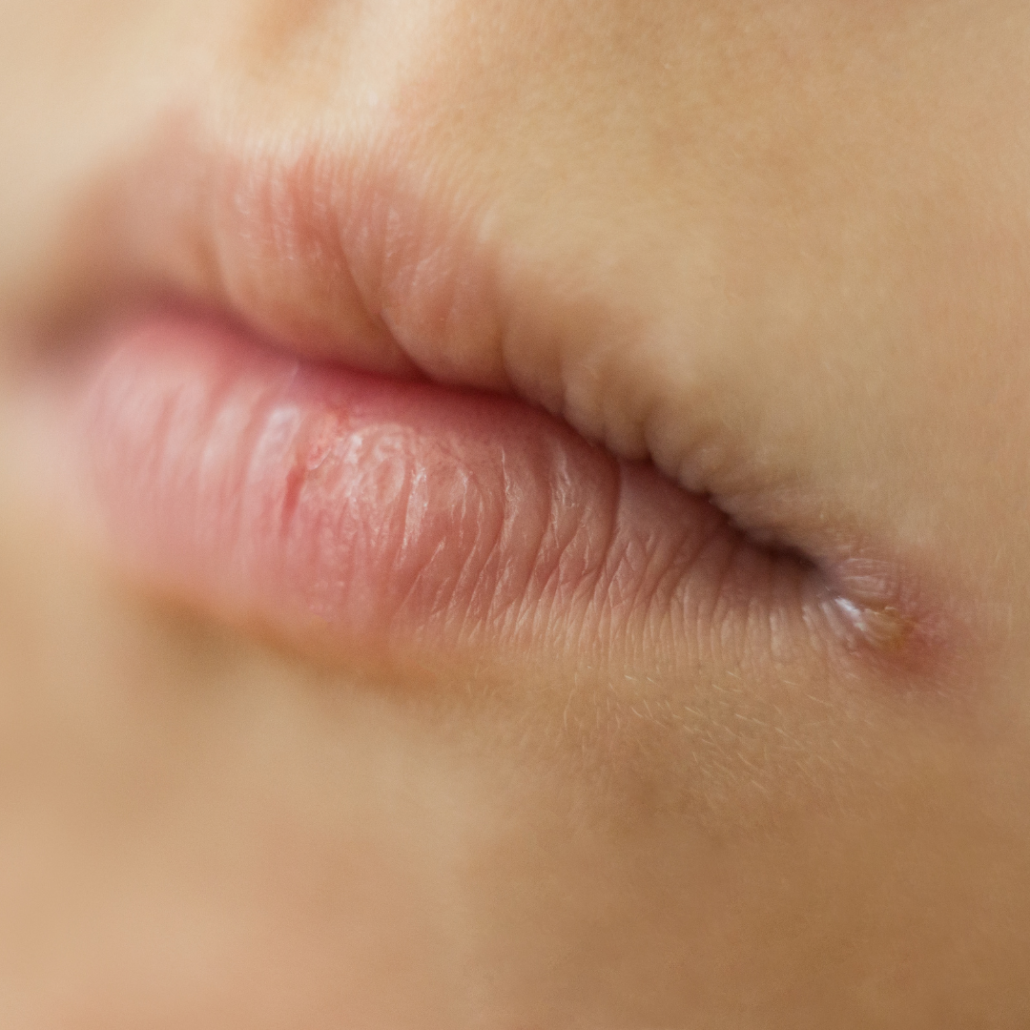
Symptoms
The corners of the mouth will nearly always show signs of this condition. Painful symptoms might range from minor redness to open, bleeding blisters. Additionally, the corners of your mouth could be anything of the following if you have angular cheilitis:
- Bleeding
- Red in color
- Swollen
- Cracked
- Blistered
- Crusty
- Itchy
- Painful
Other angular cheilitis signs and symptoms can include:
- Oral yeast infection (throat)
- Eczema-like rash on the lower face
- Redness in the mouth’s palate in those who wear dentures
- Saliva at the mouth’s corners is found in deep fissures
How is angular cheilitis diagnosed?
A physician or dermatologist will often make the diagnosis of angular cheilitis. Your doctor will inspect your mouth and other areas of your body for any possible skin irritations. They will analyse your personal and family medical histories and inquire about your lifestyle, drugs, and prescriptions. Your doctor might opt to take culture swabs from your mouth to submit to a lab since this condition can be a sign of a bacterial or fungal infection. This, however, is often only carried out in cases where other treatments have failed.
What is the treatment?

The determination of your course of treatment is led by the cause of your angular cheilitis. It could contain:
- Antibiotics: These drugs work to cure bacterial infections when used topically or orally.
- Dental work: Any oral hardware, including dentures, should fit comfortably. With braces, retainers, or headgear, crooked teeth or a bad bite may get better.
- Changes in nutrition: Eating meals high in protein, iron, and B vitamins help solve issues brought on by a bad diet or a deficiency in nutrients.
- Ointments or creams: Topical steroids or antifungal creams reduce swelling and discomfort caused by cracked corners of the mouth. You can protect and hydrate your mouth by using petroleum jelly or lip balm.
Living with angular cheilitis
In most cases, this condition is not dangerous. After beginning medication, the illness frequently gets better in approximately two weeks. If severe angular cheilitis is not treated, it may leave scars or result in fragile, thin skin. After treatment, it can reappear. The condition is chronic (ongoing) for some people. They might spend the rest of their lives managing the illness.
You can lessen pain and swelling while treating the underlying cause of angular cheilitis by:
- The corners of your mouth with ice or a cool compress.
- Avoiding skin irritants including hot foods, mouthwash, and abrasive toothpaste.
- Avoiding the sun, extremely cold weather, and wind.
- Using lip balm or ointments to keep your mouth’s corners moisturized.
For more information and treatment, contact us at Travocure.